Abstract
Objective
Lean processes involve streamlining methods and maximizing efficiency. Well established in the manufacturing industry, they are increasingly being applied to health care. The objective of this study was to determine feasibility and effectiveness of applying Lean principles to an academic medical center colonoscopy unit.
Methods
Lean process improvement involved training endoscopy personnel, observing patients, mapping the value stream, analyzing patient flow, designing and implementing new processes, and finally re-observing the process. Our primary endpoint was total colonoscopy time (minutes from check-in to discharge) with secondary endpoints of individual segment times and unit colonoscopy capacity.
Results
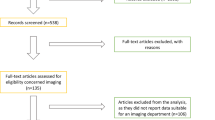
A total of 217 patients were included (November 2013–May 2014), with 107 pre-Lean and 110 post-Lean intervention. Pre-Lean total colonoscopy time was 134 min. After implementation of the Lean process, mean colonoscopy time decreased by 10 % to 121 min (p = 0.01). The three steps of the process affected by the Lean intervention (time to achieve adequate sedation, time to recovery, and time to discharge) decreased from 3.7 to 2.4 min (p < 0.01), 4.0 to 3.4 min (p = 0.09), and 41.2 to 35.4 min (p = 0.05), respectively. Overall, unit capacity of colonoscopies increased from 39.6 per day to 43.6. Post-Lean patient satisfaction surveys demonstrated an average score of 4.5/5.0 (n = 73) regarding waiting time, 4.9/5.0 (n = 60) regarding how favorably this experienced compared to prior colonoscopy experiences, and 4.9/5.0 (n = 74) regarding professionalism of staff. One hundred percentage of respondents (n = 69) stated they would recommend our institution to a friend for colonoscopy.
Discussion
With no additional utilization of resources, a single Lean process improvement cycle increased productivity and capacity of our colonoscopy unit. We expect this to result in increased patient access and revenue while maintaining patient satisfaction. We believe these results are widely generalizable to other colonoscopy units as well as other process-based interventions in health care.


Similar content being viewed by others
References
Brenner H, Chang-Claude J, Seiler CM, Sturmer T, Hoffmeister M (2007) Potential for colorectal cancer prevention of sigmoidoscopy versus colonoscopy: population-based case control study. Cancer Epidemiol Biomarkers Prev 16(3):494–499
American Cancer Society (2011) Colorectal cancer facts & figures 2011–2013. http://www.cancer.org/acs/groups/content/@epidemiologysurveilance/documents/document/acspc-028312.pdf. Accessed 14 June 2015
Harders M, Malangoni MA, Weight S, Sidhu T (2006) Improving operating room efficiency through process redesign. Am J Surg 140:509–516
Krafcik JF (1988) Triumph of the lean production system. Sloan Manage Rev 30(1):41–52
D’Andreamatteo A, Ianni L, Lega F, Sargiacomo M (2015) Lean in healthcare: a comprehensive review. Health Policy. doi:10.1016/j.healthpol.2015.02.002
Mason SE, Nicolay CR, Darzi A (2015) The use of lean and six sigma methodologies in surgery: a systematic review. Surgeon 13:91–100
Cima RR, Brown MJ, Hebl JR, Moore R, Rogers JC, Kollengode A, Amstutz GJ, Weisbrod CA, Narr BJ, Deschamps C (2011) Use of lean and six sigma methodology to improve operating room efficiency in a high-volume tertiary-care academic medical center. J Am Coll Surg 213:83–92 (discussion 93–94)
Toussaint JS, Berry LL (2013) The promise of lean in healthcare. Mayo Clin Proc 88(1):74–82
Mandel JE, Tanner JW, Lichtenstein GR, Metz DC, Katzka DA, Ginsberg GG, Kochman ML (2007) A randomized, double-blind trial of patient-controlled sedation with propofol/remifentanil versus midazolam/fentanyl for colonoscopy. Anesth Analg 106(2):434–439
Vargo JJ, Bramley T, Meyer K, Nightengale B (2007) Practice efficiency and economics: the case for rapid recovery sedation agents for colonoscopy in a screening population. J Clin Gastroenterol 41(6):591–598
Dickson EW, Singh S, Cheung DS, Wyatt CC, Nugent AS (2009) Application of lean manufacturing techniques in the emergency department. J Emerg Med 37(2):177–182
Collar RM, Shuman AG, Feiner S, McGonegal AK, Heidel N, Duck M, McLean SA, Billi JE, Healy DW, Bradford CR (2012) Lean management in academic surgery. J Am Coll Surg 214:928–936
Chapman F (2009) Practice Management. Highlights of 2009 ASGE endoscopic operations survey. ASGE News March/April 29–30. http://www.asge.org/uploadedfiles/asge_news/asgenewsmarch10.pdf
Holden RJ (2010) Lean thinking in emergency departments: a critical review. Ann Emerg Med 57:265–278
Delisle DR (2015) Executing lean improvements: a practical guide with real-world healthcare studies. ASQ Quality Quality Press, Milwaukee
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Damle, Mr. Andrew, Drs. Kaur, Orquiola, Alavi, Steele, and Maykel have no conflict of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Damle, A., Andrew, N., Kaur, S. et al. Elimination of waste: creation of a successful Lean colonoscopy program at an academic medical center. Surg Endosc 30, 3071–3076 (2016). https://doi.org/10.1007/s00464-015-4599-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-015-4599-6