Abstract
Purpose
Patterns of locoregional rectal cancer recurrences following total mesorectal excision (TME) were analyzed to define the irradiation volume, especially the lateral pelvic lymph node (LPLN).
Materials and methods
Of 1243 patients who underwent TME without pelvic radiotherapy between 2005 and 2012, the data of 826 patients with rectal adenocarcinoma without distant metastases were analyzed for relapse patterns, categorized as distant and locoregional (anastomosis, mesorectum, presacral area, and LPLNs) failure.
Results
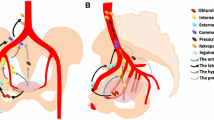
The median follow-up was 61.8 months. The 5-year local recurrence-free, distant metastasis-free, overall survival rates were 88, 82, and 89%, respectively. Relapse occurred in 108 (13%) patients: 90 (11%) had distant and 28 (3%) had locoregional failure. Eight patients had LPLN recurrence: the 2 recurrences from upper rectal cancers occurred near the bifurcation of the common iliac artery into the external and internal iliac vessels; the 6 mid-lower rectal cancers had 16 recurrences near the internal iliac and obturator arteries—five occurred anterior to the obturator artery and posterior to the external iliac artery, superior to the femoral head. LPLN recurrence was associated with pN2 stage, perinodal extension, and lymphovascular invasion.
Conclusion
The LPLN component of pre- or postoperative irradiation volumes could potentially be optimized based on our mapping data. However, since patients in our institution at high risk for relapse received either preoperative or postoperative chemoradiation, further analyses are needed to confirm our findings.


Similar content being viewed by others
References
Akiyoshi T, Watanabe T, Miyata S, Kotake K, Muto T, Sugihara K, Japanese Society for Cancer of the C, Rectum (2012) Results of a Japanese nationwide multi-institutional study on lateral pelvic lymph node metastasis in low rectal cancer: is it regional or distant disease?. Ann Surg 255(6):1129–1134
Chang JS, Lee Y, Lim JS, Kim NK, Baik SH, Min BS, Huh H, Koom WS (2014) The magnetic resonance imaging-based approach for identification of high-risk patients with upper rectal cancer. Ann Surg 260(2):293–298
Choi SH, Chang JS, Kim NK, Lim JS, Min BS, Hur H, Shin SJ, Ahn JB, Kim YB, Koom WS (2017) Reduced pelvic field sparing anastomosis for postoperative radiotherapy in selected patients with mid-upper rectal cancer. J Radiat Res. https://doi.org/10.1093/jrr/rrw127
El-Malt M, Ceelen W, De Meerleer G, Verstraete A, Boterberg T, Van Belle S, de Hemptinne B, De Neve W, Pattyn P (2001) Influence of preoperative combined radiochemotherapy on surgical outcome and colonic anastomotic healing: experimental study in the rat. Int J Radiat Oncol Biol Phys 50(4):1073–1078
Fujita S, Akasu T, Mizusawa J et al (2012) Postoperative morbidity and mortality after mesorectal excision with and without lateral lymph node dissection for clinical stage II or stage III lower rectal cancer (JCOG0212): results from a multicentre, randomised controlled, non-inferiority trial. Lancet Oncol 13(6):616–621
Fujita S, Mizusawa J, Kanemitsu Y et al (2017) Mesorectal excision with or without lateral lymph node dissection for clinical Stage II/III lower rectal cancer (JCOG0212): a multicenter, randomized controlled, noninferiority trial. Ann Surg 266(2):201–207
Fuller CD, Nijkamp J, Duppen JC et al (2011) Prospective randomized double-blind pilot study of site-specific consensus atlas implementation for rectal cancer target volume delineation in the cooperative group setting. Int J Radiat Oncol Biol Phys 79(2):481–489
Georgiou P, Tan E, Gouvas N, Antoniou A, Brown G, Nicholls RJ, Tekkis P (2009) Extended lymphadenectomy versus conventional surgery for rectal cancer: a meta-analysis. Lancet Oncol 10(11):1053–1062
Group MS, Shihab OC, Taylor F et al (2011) Relevance of magnetic resonance imaging-detected pelvic sidewall lymph node involvement in rectal cancer. Br J Surg 98(12):1798–1804
Gunderson LL, Sargent DJ, Tepper JE et al (2004) Impact of T and N stage and treatment on survival and relapse in adjuvant rectal cancer: a pooled analysis. J Clin Oncol 22(10):1785–1796
Hassan I, Larson DW, Wolff BG, Cima RR, Chua HK, Hahnloser D, O’Byrne MM, Larson DR, Pemberton JH (2008) Impact of pelvic radiotherapy on morbidity and durability of sphincter preservation after coloanal anastomosis for rectal cancers. Dis Colon Rectum 51(1):32–37
Japanese Research Society for Cancer of the Colon and Rectum (1983) General rules for clinical and pathological studies on cancer of the colon, rectum and anus. Part II. Histopathological classification. Jpn J Surg 13(6):574–598
Kim TH, Jeong SY, Choi DH, Kim DY, Jung KH, Moon SH, Chang HJ, Lim SB, Choi HS, Park JG (2008) Lateral lymph node metastasis is a major cause of locoregional recurrence in rectal cancer treated with preoperative chemoradiotherapy and curative resection. Ann Surg Oncol 15(3):729–737
Kim MS, Keum KC, Rhee WJ, Kim H, Kim M, Choi S, Nam KC, Koom WS (2013) The location of locoregional recurrence in pathologic T3N0, non-irradiated lower rectal cancer. Radiat Oncol J 31(2):97–103
Kim TG, Park W, Choi DH et al (2014) Factors associated with lateral pelvic recurrence after curative resection following neoadjuvant chemoradiotherapy in rectal cancer patients. Int J Colorectal Dis 29(2):193–200
Kusters M, Marijnen CA, van de Velde CJ, Rutten HJ, Lahaye MJ, Kim JH, Beets-Tan RG, Beets GL (2010) Patterns of local recurrence in rectal cancer; a study of the Dutch TME trial. Eur J Surg Oncol 36(5):470–476
Nijkamp J, Kusters M, Beets-Tan RG, Martijn H, Beets GL, van de Velde CJ, Marijnen CA (2011) Three-dimensional analysis of recurrence patterns in rectal cancer: the cranial border in hypofractionated preoperative radiotherapy can be lowered. Int J Radiat Oncol Biol Phys 80(1):103–110
Pahlman L, Bohe M, Cedermark B, Dahlberg M, Lindmark G, Sjodahl R, Ojerskog B, Damber L, Johansson R (2007) The Swedish rectal cancer registry. Br J Surg 94(10):1285–1292
Roels S, Duthoy W, Haustermans K, Penninckx F, Vandecaveye V, Boterberg T, De Neve W (2006) Definition and delineation of the clinical target volume for rectal cancer. Int J Radiat Oncol Biol Phys 65(4):1129–1142
Sauer R, Becker H, Hohenberger W et al (2004) Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med 351(17):1731–1740
Steup WH, Moriya Y, van de Velde CJ (2002) Patterns of lymphatic spread in rectal cancer. A topographical analysis on lymph node metastases. Eur J Cancer 38(7):911–918
Sugihara K, Kobayashi H, Kato T, Mori T, Mochizuki H, Kameoka S, Shirouzu K, Muto T (2006) Indication and benefit of pelvic sidewall dissection for rectal cancer. Dis Colon Rectum 49(11):1663–1672
Syk E, Torkzad MR, Blomqvist L, Ljungqvist O, Glimelius B (2006) Radiological findings do not support lateral residual tumour as a major cause of local recurrence of rectal cancer. Br J Surg 93(1):113–119
Valentini V, Gambacorta MA, Barbaro B et al (2016) International consensus guidelines on clinical target volume delineation in rectal cancer. Radiother Oncol 120(2):195–201
van Gijn W, Marijnen CA, Nagtegaal ID et al (2011) Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer: 12-year follow-up of the multicentre, randomised controlled TME trial. Lancet Oncol 12(6):575–582
Watanabe T, Itabashi M, Shimada Y et al (2015) Japanese Society for Cancer of the Colon and Rectum (JSCCR) Guidelines 2014 for treatment of colorectal cancer. Int J Clin Oncol 20(2):207–239
Wei M, Wu Q, Fan C, Li Y, Chen X, Zhou Z, Han J, Wang Z (2016) Lateral pelvic lymph node dissection after neoadjuvant chemo-radiation for preoperative enlarged lateral nodes in advanced low rectal cancer: study protocol for a randomized controlled trial. Trials 17(1):561
Funding
This work was supported by the National Research Foundation of Korea (NRF) Grant, funded by the Korean government (MSIP) (NRF-2015R1D1A1A01060710).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have stated that they have no conflicts of interest.
Research involving human participants and/or animals
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, informed consent is not required.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Choi, S.H., Chang, J.S., Yoon, H.I. et al. Mapping of lateral pelvic lymph node recurrences in rectal cancer: a radiation oncologist’s perspective. J Cancer Res Clin Oncol 144, 1119–1128 (2018). https://doi.org/10.1007/s00432-018-2624-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-018-2624-6