Abstract
Purpose
To analyze potential alterations in corneal nerve morphology and function in different stages of Fuchs’ endothelial corneal dystrophy (FECD).
Methods
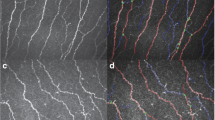
Thirty eyes with FECD underwent in vivo confocal microscopy using the Heidelberg Retina Tomograph II (HRT II; Heidelberg Engineering, Heidelberg, Germany) and the Rostock Cornea Module (RCM) to quantify the morphology of the central subbasal corneal nerve plexus (total nerve length, total nerve number, number of main nerve trunks, number of nerve branches) as well as esthesiometry (using the Cochet-Bonnet esthesiometer) of the central cornea to determine central corneal sensation as a measure of nerve function. Findings were correlated with an age-matched control group of 30 healthy individuals. Comparisons to biomicroscopical stage of FECD, visual acuity and central corneal thickness were performed using Spearman correlation.
Results
Depending on slit-lamp examination, all 30 eyes were classified into FECD stage 1–4 (stage 1: six eyes; stage 2: 15 eyes; stage 3: six eyes; stage 4: three eyes). Total nerve length (ρ = −0.8, p < 0.001), total nerve number (ρ = −0.7, p < 0.001), number of main nerve trunks (ρ = −0.6, p < 0.001), and number of nerve branches (ρ = −0.7, p < 0.001) decreased significantly with increasing FECD stages. Comparing to the visual acuity, significant positive correlations were found for total nerve length (ρ = 0.5, p = 0.012), total nerve number (ρ = 0.5, p = 0.005), number of main nerve trunks (ρ = 0.4, p = 0.017), and number of nerve branches (ρ = 0.5, p = 0.009). With central corneal thickness, there were significant inverse correlations for total nerve length (ρ = −0.6, p = 0.001), total nerve number (ρ = −0.5, p = 0.012), number of main nerve trunks (ρ = −0.4, p = 0.015), and number of nerve branches (ρ = −0.4, p = 0.017). Central corneal sensation was full in all FECD stage 1, stage 2 and stage 3 eyes, but mildly reduced in FECD stage 4 eyes.
Conclusions
Increasing severity of Fuchs’ endothelial corneal dystrophy (FECD) is concurrent with marked attenuation of the density, as well as mild diminishment of the function, of the subbasal corneal nerve plexus in late stage of the disease.




Similar content being viewed by others
References
Adamis AP, Filatov V, Tripathi BJ, Tripathi RC (1993) Fuchs’ endothelial dystrophy of the cornea. Surv Ophthalmol 38:149–168
Matthaei M, Hu J, Meng H, Lackner EM, Eberhart CG, Qian J, Hao H, Jun AS (2013) Endothelial cell whole genome expression analysis in a mouse model of early-onset Fuchs’ endothelial corneal dystrophy. Invest Ophthalmol Vis Sci 54:1931–1940
Matthaei M, Lackner EM, Meng H, Hicks JL, Meeker AK, Eberhart CG, Jun AS (2013) Tissue microarray analysis of cyclin-dependent kinase inhibitors p21 and p16 in Fuchs dystrophy. Cornea 32:473–478
Melles GR, Ong TS, Ververs B, van der Wees J (2006) Descemet membrane endothelial keratoplasty (DMEK). Cornea 25:987–990
Heindl LM, Hofmann-Rummelt C, Schlötzer-Schrehardt U, Kruse FE, Cursiefen C (2008) Histologic analysis of descemet stripping in posterior lamellar keratoplasty. Arch Ophthalmol 126:461–464
Heindl LM, Riss S, Bachmann BO, Laaser K, Kruse FE, Cursiefen C (2011) Split cornea transplantation for 2 recipients: a new strategy to reduce corneal tissue cost and shortage. Ophthalmology 118:294–301
Guerra FP, Anshu A, Price MO, Giebel AW, Price FW (2011) Descemet’s membrane endothelial keratoplasty: prospective study of 1-year visual outcomes, graft survival, and endothelial cell loss. Ophthalmology 118:2368–2373
Heindl LM, Riss S, Laaser K, Bachmann BO, Kruse FE, Cursiefen C (2011) Split cornea transplantation for 2 recipients—review of the first 100 consecutive patients. Am J Ophthalmol 152:523–532
Terry MA, Straiko MD, Goshe JM, Li JY, Davis-Boozer D (2012) Descemet’s stripping automated endothelial keratoplasty: the tenuous relationship between donor thickness and postoperative vision. Ophthalmology 119:1988–1996
Heindl LM, Riss S, Adler W, Bucher F, Hos D, Cursiefen C (2013) Split cornea transplantation: relationship between storage time of split donor tissue and outcome. Ophthalmology 120:899–907
Cursiefen C, Kuchle M, Naumann GO (1998) Changing indications for penetrating keratoplasty: histopathology of 1,250 corneal buttons. Cornea 17:468–470
Oliveira-Soto L, Efron N (2001) Morphology of corneal nerves using confocal microscopy. Cornea 20:374–384
Guthoff RF, Wienss H, Hahnel C, Wree A (2005) Epithelial innervation of human cornea: a three-dimensional study using confocal laser scanning fluorescence microscopy. Cornea 24:608–613
Hamrah P, Cruzat A, Dastjerdi MH, Zheng L, Shahatit BM, Bayhan HA, Dana R, Pavan-Langston D (2010) Corneal sensation and sub-basal nerve alterations in patients with herpes simplex keratitis: an in vivo confocal microscopy study. Ophthalmology 117:1930–1936
Hamrah P, Cruzat A, Dastjerdi MH, Prüss H, Zheng L, Shahatit BM, Bayhan HA, Dana R, Pavan-Langston D (2013) Unilateral herpes zoster ophthalmicus results in bilateral corneal nerve alteration: an in vivo confocal microscopy study. Ophthalmology 120:40–47
Patel DV, McGhee CN (2009) In vivo confocal microscopy of human corneal nerves in health, in ocular and systemic disease, and following corneal surgery: a review. Br J Ophthalmol 93:853–860
Cruzat A, Pavan-Langston D, Hamrah P (2010) In vivo confocal microscopy of corneal nerves: analysis and clinical correlation. Semin Ophthalmol 25:171–177
Alhatem A, Cavalcanti B, Hamrah P (2012) In vivo confocal microscopy in dry eye disease and related conditions. Semin Ophthalmol 27:138–148
Kurbanyan K, Hoesl LM, Schrems WA, Hamrah P (2012) Corneal nerve alterations in acute Acanthamoeba and fungal keratitis: an in vivo confocal microscopy study. Eye 26:126–132
Schrems-Hoesl LM, Schrems WA, Cruzat A, Shahatit BM, Bayhan HA, Jurkunas UV, Hamrah P (2013) Cellular and sub-basal nerve alterations in early stage Fuchs’ endothelial corneal dystrophy: an in vivo confocal microscopy study. Eye 27:42–49
Meijering E, Jacob M, Sarria JC, Steiner P, Hirling H, Unser M (2004) Design and validation of a tool for neurite tracing and analysis in fluorescence microscopy images. Cytometry A 58:167–176
Chiou AG, Kaufman SC, Beuerman RW, Ohta T, Soliman H, Kaufman HE (1999) Confocal microscopy in cornea guttata and Fuchs’ endothelial dystrophy. Br J Ophthalmol 83:185–189
Mustonen RK, McDonald MB, Srivannaboon S, Tan AL, Doubrava MW, Kim CK (1998) In vivo confocal microscopy of Fuchs’ endothelial dystrophy. Cornea 17:493–503
Hara M, Morishige N, Chikama T, Nishida T (2003) Comparison of confocal biomicroscopy and noncontact specular microscopy for evaluation of the corneal endothelium. Cornea 22:512–515
Koh SW, Waschek JA (2000) Corneal endothelial cell survival in organ cultures under oxidative stress: effect of VIP. Invest Ophthalmol Vis Sci 41:4085–4092
Koh SW, Chandrasekara K, Abbondandolo CJ, Coll TJ, Rutzen AR (2008) VIP and VIP gene silencing modulation of differentiation marker N-cadherin and cell shape of corneal endothelium in human corneas ex vivo. Invest Ophthalmol Vis Sci 49:3491–3498
Sornelli F, Lambiase A, Mantelli F, Aloe L (2010) NGF and NGF-receptor expression of cultured immortalized human corneal endothelial cells. Molecular vision 16:1439–1447
Zhu AY, Eberhart CG, Jun AS (2014) Fuchs endothelial corneal dystrophy: a neurodegenerative disorder? JAMA Ophthalmol 2013:7993
Cursiefen C, Seitz B, Kruse FE (2005) Neurotrophic keratitis. Ophthalmologe 102:7–14
Financial support
German Research Foundation (HE 6743/2-1 to L.M.H.; STE 1928/2-1 to P.S.; Priority Research Project SFB 643: B10, CU 47/6-1, CU 47/4-1 to C.C.); GEROK-Programme University Hospital of Cologne (to F.B., L.M.H. and D.H.); EU FP7 STRONG (F.B.; C.C.); Ruth and Helmut Lingen Foundation, Cologne.
Conflict of interest
None of the authors has a financial or proprietary interest in any material or method mentioned in the manuscript. All authors have full control of all primary data and they agree to allow Graefes Archive for Clinical and Experimental Ophthalmology to review their data upon request.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bucher, F., Adler, W., Lehmann, H.C. et al. Corneal nerve alterations in different stages of Fuchs’ endothelial corneal dystrophy: an in vivo confocal microscopy study. Graefes Arch Clin Exp Ophthalmol 252, 1119–1126 (2014). https://doi.org/10.1007/s00417-014-2678-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-014-2678-3