Abstract
Purpose
Intelligence has a strong influence on life capability, and thus, identifying early modifiable risk factors related to cognitive ability is of major public health interest. During pregnancy, vitamin D is transported from the mother to the fetus through the placenta in the form of 25-hydroxyvitamin D (25(OH)D). Levels of 25(OH)D have in some studies been associated with childhood neurodevelopment; however, results from all studies are not in agreement. We investigated if neonatal 25(OH)D3 concentrations were associated with Børge Priens IQ test score (BPP) in young adulthood.
Methods
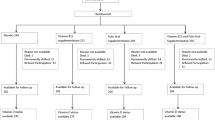
In this nested cohort study, 25(OH)D3 concentrations were measured in dried blood spots from 818 newborns. We followed the children for their IQ BPP test scores in the Danish Conscription Register, which holds information on test results from the BPP test on individuals who have been recruited for Danish mandatory military draft board examination. Using general linear models, we investigated the crude and adjusted relationship between quintiles of 25(OH)D3 concentrations and BPP IQ test results.
Results
The study population consisted of 95.8% men, with a mean age of 19.4 years. The median and range of the neonatal 25(OH)D3 levels were 26.2 nmol/L (0–104.7 nmol/L). The overall Wald test did not show an association between neonatal 25(OH)D3 levels and BPP IQ scores (p = 0.23); however, individuals within the 3rd (BPP IQ = 101.0, 98.0–103.9) and 4th (BPP IQ = 101.2, 99.1–104.3) quintiles had slightly higher BPP IQ scores than individuals from the first quintile (BPP IQ = 97.6, 94.6–100.6).
Conclusions
Our results support the hypothesis that individuals with the lowest levels of neonatal vitamin D might have slightly lower BPP. However, more studies are needed with larger study populations to confirm our results.
Similar content being viewed by others
References
Tau GZ, Peterson BS (2010) Normal development of brain circuits. Neuropsychopharmacology 35(1):147–168. https://doi.org/10.1038/npp.2009.115
Stiles J, Jernigan TL (2010) The basics of brain development. Neuropsychol Rev 20(4):327–348. https://doi.org/10.1007/s11065-010-9148-4
Ackerman S (1992) Discovering the brain. National Academies Press, Washington, DC. https://doi.org/10.17226/1785(Copyright (c) 1992 by the National Academy of Sciences)
Cass WA, Peters LE, Fletcher AM, Yurek DM (2012) Evoked dopamine overflow is augmented in the striatum of calcitriol treated rats. Neurochem Int 60(2):186–191. https://doi.org/10.1016/j.neuint.2011.11.010
Patrick RP, Ames BN (2014) Vitamin D hormone regulates serotonin synthesis. Part 1: relevance for autism. FASEB J 28(6):2398–2413. https://doi.org/10.1096/fj.13-246546
Watanabe M, Maemura K, Kanbara K, Tamayama T, Hayasaki H (2002) GABA and GABA receptors in the central nervous system and other organs. Int Rev Cytol 213:1–47
Gaspar P, Cases O, Maroteaux L (2003) The developmental role of serotonin: news from mouse molecular genetics. Nat Rev Neurosci 4(12):1002–1012. https://doi.org/10.1038/nrn1256
Patrick RP, Ames BN (2015) Vitamin D and the omega-3 fatty acids control serotonin synthesis and action, part 2: relevance for ADHD, bipolar disorder, schizophrenia, and impulsive behavior. FASEB J 29(6):2207–2222. https://doi.org/10.1096/fj.14-268342
Jiang P, Zhang LH, Cai HL, Li HD, Liu YP, Tang MM, Dang RL, Zhu WY, Xue Y, He X (2014) Neurochemical effects of chronic administration of calcitriol in rats. Nutrients 6(12):6048–6059. https://doi.org/10.3390/nu6126048
Neveu I, Naveilhan P, Jehan F, Baudet C, Wion D, De Luca HF, Brachet P (1994) 1,25-Dihydroxyvitamin D3 regulates the synthesis of nerve growth factor in primary cultures of glial cells. Brain Res Mol Brain Res 24(1–4):70–76
Verity AN, Wyatt TL, Lee W, Hajos B, Baecker PA, Eglen RM, Johnson RM (1999) Differential regulation of glial cell line-derived neurotrophic factor (GDNF) expression in human neuroblastoma and glioblastoma cell lines. J Neurosci Res 55(2):187–197. https://doi.org/10.1002/(sici)1097-4547(19990115)55:2%3c187:aid-jnr6%3e3.0.co;2-t
Koo H, Choi BH (2001) Expression of glial cell line-derived neurotrophic factor (GDNF) in the developing human fetal brain. Int J Dev Neurosci 19(6):549–558
Murthi P, Davies-Tuck M, Lappas M, Singh H, Mockler J, Rahman R, Lim R, Leaw B, Doery J, Wallace EM, Ebeling PR (2017) Maternal 25-hydroxyvitamin D is inversely correlated with foetal serotonin. Clin Endocrinol (Oxf) 86(3):401–409. https://doi.org/10.1111/cen.13281
Eyles D, Burne T, McGrath J (2011) Vitamin D in fetal brain development. Semin Cell Dev Biol 22(6):629–636. https://doi.org/10.1016/j.semcdb.2011.05.004
Pet MA, Brouwer-Brolsma EM (2016) The impact of maternal vitamin d status on offspring brain development and function: a systematic review. Adv Nutr (Bethesda, MD) 7(4):665–678. https://doi.org/10.3945/an.115.010330
Zakon HH (1998) The effects of steroid hormones on electrical activity of excitable cells. Trends Neurosci 21(5):202–207
Srivastava DP, Waters EM, Mermelstein PG, Kramar EA, Shors TJ, Liu F (2011) Rapid estrogen signaling in the brain: implications for the fine-tuning of neuronal circuitry. J Neurosci 31(45):16056–16063. https://doi.org/10.1523/jneurosci.4097-11.2011
Chklovskii DB, Mel BW, Svoboda K (2004) Cortical rewiring and information storage. Nature 431(7010):782–788. https://doi.org/10.1038/nature03012
Garcion E, Nataf S, Berod A, Darcy F, Brachet P (1997) 1,25-Dihydroxyvitamin D3 inhibits the expression of inducible nitric oxide synthase in rat central nervous system during experimental allergic encephalomyelitis. Brain Res Mol Brain Res 45(2):255–267
Eyles DW, Smith S, Kinobe R, Hewison M, McGrath JJ (2005) Distribution of the vitamin D receptor and 1 alpha-hydroxylase in human brain. J Chem Neuroanat 29(1):21–30. https://doi.org/10.1016/j.jchemneu.2004.08.006
Garcion E, Sindji L, Montero-Menei C, Andre C, Brachet P, Darcy F (1998) Expression of inducible nitric oxide synthase during rat brain inflammation: regulation by 1,25-dihydroxyvitamin D3. Glia 22(3):282–294
Ibi M, Sawada H, Nakanishi M, Kume T, Katsuki H, Kaneko S, Shimohama S, Akaike A (2001) Protective effects of 1 alpha,25-(OH)(2)D(3) against the neurotoxicity of glutamate and reactive oxygen species in mesencephalic culture. Neuropharmacology 40(6):761–771
de Viragh PA, Haglid KG, Celio MR (1989) Parvalbumin increases in the caudate putamen of rats with vitamin D hypervitaminosis. Proc Natl Acad Sci USA 86(10):3887–3890
Brewer LD, Thibault V, Chen KC, Langub MC, Landfield PW, Porter NM (2001) Vitamin D hormone confers neuroprotection in parallel with downregulation of l-type calcium channel expression in hippocampal neurons. J Neurosci 21(1):98–108
Dursun E, Gezen-Ak D, Yilmazer S (2011) A novel perspective for Alzheimer’s disease: vitamin D receptor suppression by amyloid-beta and preventing the amyloid-beta induced alterations by vitamin D in cortical neurons. J Alzheimers Dis JAD 23(2):207–219. https://doi.org/10.3233/jad-2010-101377
Benros ME, Sorensen HJ, Nielsen PR, Nordentoft M, Mortensen PB, Petersen L (2015) The association between infections and general cognitive ability in young men—a nationwide study. PLoS One 10(5):e0124005. https://doi.org/10.1371/journal.pone.0124005
Gimeno D, Marmot MG, Singh-Manoux A (2008) Inflammatory markers and cognitive function in middle-aged adults: the Whitehall II study. Psychoneuroendocrinology 33(10):1322–1334. https://doi.org/10.1016/j.psyneuen.2008.07.006
Darling AL, Rayman MP, Steer CD, Golding J, Lanham-New SA, Bath SC (2017) Association between maternal vitamin D status in pregnancy and neurodevelopmental outcomes in childhood: results from the Avon Longitudinal Study of Parents and Children (ALSPAC). Br J Nutr 117(12):1682–1692. https://doi.org/10.1017/s0007114517001398
Hanieh S, Ha TT, Simpson JA, Thuy TT, Khuong NC, Thoang DD, Tran TD, Tuan T, Fisher J, Biggs BA (2014) Maternal vitamin D status and infant outcomes in rural Vietnam: a prospective cohort study. PLoS One 9(6):e99005. https://doi.org/10.1371/journal.pone.0099005
Chawla D, Fuemmeler B, Benjamin-Neelon SE, Hoyo C, Murphy S, Daniels JL (2017) Early prenatal vitamin D concentrations and social–emotional development in infants. J Maternal Fetal Neonatal Med. https://doi.org/10.1080/14767058.2017.1408065
Gould JF, Anderson AJ, Yelland LN, Smithers LG, Skeaff CM, Zhou SJ, Gibson RA, Makrides M (2017) Association of cord blood vitamin D with early childhood growth and neurodevelopment. J Paediatr Child Health 53(1):75–83. https://doi.org/10.1111/jpc.13308
Tylavsky FA, Kocak M, Murphy LE, Graff JC, Palmer FB, Volgyi E, Diaz-Thomas AM, Ferry RJ Jr (2015) Gestational vitamin 25(OH)d status as a risk factor for receptive language development: a 24-month, longitudinal, observational study. Nutrients 7(12):9918–9930. https://doi.org/10.3390/nu7125499
Whitehouse AJ, Holt BJ, Serralha M, Holt PG, Kusel MM, Hart PH (2012) Maternal serum vitamin D levels during pregnancy and offspring neurocognitive development. Pediatrics 129(3):485–493. https://doi.org/10.1542/peds.2011-2644
Zhu P, Tong SL, Hao JH, Tao RX, Huang K, Hu WB, Zhou QF, Jiang XM, Tao FB (2015) Cord blood vitamin D and neurocognitive development are nonlinearly related in toddlers. J Nutr 145(6):1232–1238. https://doi.org/10.3945/jn.114.208801
Laird E, Thurston SW, van Wijngaarden E, Shamlaye CF, Myers GJ, Davidson PW, Watson GE, McSorley EM, Mulhern MS, Yeates AJ, Ward M, McNulty H, Strain JJ (2017) Maternal vitamin D status and the relationship with neonatal anthropometric and childhood neurodevelopmental outcomes: results from the seychelles child development nutrition study. Nutrients. https://doi.org/10.3390/nu9111235
Keim SA, Bodnar LM, Klebanoff MA (2014) Maternal and cord blood 25(OH)-vitamin D concentrations in relation to child development and behaviour. Paediatr Perinat Epidemiol 28(5):434–444. https://doi.org/10.1111/ppe.12135
Daraki V, Roumeliotaki T, Koutra K, Chalkiadaki G, Katrinaki M, Kyriklaki A, Kampouri M, Margetaki K, Vafeiadi M, Papavasiliou S, Kogevinas M, Chatzi L (2018) High maternal vitamin D levels in early pregnancy may protect against behavioral difficulties at preschool age: the Rhea mother–child cohort, Crete, Greece. Eur Child Adolesc Psychiatry 27(1):79–88. https://doi.org/10.1007/s00787-017-1023-x
McCarthy EK, Murray DM, Malvisi L, Kenny LC, Hourihane JOB, Irvine AD, Kiely ME (2018) Antenatal vitamin D status is not associated with standard neurodevelopmental assessments at age 5 years in a well-characterized prospective maternal–infant cohort. J Nutr 148(10):1580–1586. https://doi.org/10.1093/jn/nxy150
Gale CR, Robinson SM, Harvey NC, Javaid MK, Jiang B, Martyn CN, Godfrey KM, Cooper C (2008) Maternal vitamin D status during pregnancy and child outcomes. Eur J Clin Nutr 62(1):68–77. https://doi.org/10.1038/sj.ejcn.1602680
Veena SR, Krishnaveni GV, Srinivasan K, Thajna KP, Hegde BG, Gale CR, Fall CH (2017) Association between maternal vitamin D status during pregnancy and offspring cognitive function during childhood and adolescence. Asia Pac J Clin Nutr 26(3):438–449. https://doi.org/10.6133/apjcn.032016.07
Strom M, Halldorsson TI, Hansen S, Granstrom C, Maslova E, Petersen SB, Cohen AS, Olsen SF (2014) Vitamin D measured in maternal serum and offspring neurodevelopmental outcomes: a prospective study with long-term follow-up. Ann Nutr Metab 64(3–4):254–261. https://doi.org/10.1159/000365030
Jacobsen R, Abrahamsen B, Bauerek M, Holst C, Jensen CB, Knop J, Raymond K, Rasmussen LB, Stougaard M, Sorensen TI, Vaag AA, Heitmann BL (2013) The influence of early exposure to vitamin D for development of diseases later in life. BMC Public Health 13:515. https://doi.org/10.1186/1471-2458-13-515
Norgaard-Pedersen B, Hougaard DM (2007) Storage policies and use of the Danish Newborn Screening Biobank. J Inherit Metab Dis 30(4):530–536. https://doi.org/10.1007/s10545-007-0631-x
Eyles D, Anderson C, Ko P, Jones A, Thomas A, Burne T, Mortensen PB, Norgaard-Pedersen B, Hougaard DM, McGrath J (2009) A sensitive LC/MS/MS assay of 25OH vitamin D3 and 25OH vitamin D2 in dried blood spots. Clin Chim Acta 403(1–2):145–151. https://doi.org/10.1016/j.cca.2009.02.005
Jacobsen R, Thorsen SU, Cohen AS, Lundqvist M, Frederiksen P, Pipper CB, Pociot F, Thygesen LC, Ascherio A, Svensson J, Heitmann BL (2016) Neonatal vitamin D status is not associated with later risk of type 1 diabetes: results from two large Danish population-based studies. Diabetologia 59(9):1871–1881. https://doi.org/10.1007/s00125-016-4002-8
Handel MN, Frederiksen P, Cohen A, Cooper C, Heitmann BL, Abrahamsen B (2017) Neonatal vitamin D status from archived dried blood spots and future risk of fractures in childhood: results from the D-tect study, a population-based case-cohort study. Am J Clin Nutr 106(1):155–161. https://doi.org/10.3945/ajcn.116.145599
Kayiran SM, Ozbek N, Turan M, Gurakan B (2003) Significant differences between capillary and venous complete blood counts in the neonatal period. Clin Lab Haematol 25(1):9–16
Salle BL, Glorieux FH, Delvin EE (1988) Perinatal vitamin D metabolism. Biol Neonate 54(4):181–187
Jones KS, Assar S, Harnpanich D, Bouillon R, Lambrechts D, Prentice A, Schoenmakers I (2014) 25(OH)D2 half-life is shorter than 25(OH)D3 half-life and is influenced by DBP concentration and genotype. J Clin Endocrinol Metab 99(9):3373–3381. https://doi.org/10.1210/jc.2014-1714
Teasdale TW (2009) The Danish draft board’s intelligence test, Borge Priens Prove: psychometric properties and research applications through 50 years. Scand J Psychol 50(6):633–638. https://doi.org/10.1111/j.1467-9450.2009.00789.x
Hypponen E, Power C (2007) Hypovitaminosis D in British adults at age 45 y: nationwide cohort study of dietary and lifestyle predictors. Am J Clin Nutr 85(3):860–868. https://doi.org/10.1093/ajcn/85.3.860
Smith CA, Sun C, Pezic A, Rodda C, Cameron F, Allen K, Craig ME, Carlin J, Dwyer T, Lucas RM, Eyles DW, Kemp AS, Ellis JA, Ponsonby AL (2017) Determinants of neonatal vitamin D levels as measured on neonatal dried blood spot samples. Neonatology 111(2):153–161. https://doi.org/10.1159/000448680
Moody L, Chen H, Pan YX (2017) Early-life nutritional programming of cognition—the fundamental role of epigenetic mechanisms in mediating the relation between early-life environment and learning and memory process. Adv Nutr (Bethesda, Md) 8(2):337–350. https://doi.org/10.3945/an.116.014209
Veena SR, Gale CR, Krishnaveni GV, Kehoe SH, Srinivasan K, Fall CH (2016) Association between maternal nutritional status in pregnancy and offspring cognitive function during childhood and adolescence; a systematic review. BMC Pregnancy Childbirth 16:220. https://doi.org/10.1186/s12884-016-1011-z
Basatemur E, Gardiner J, Williams C, Melhuish E, Barnes J, Sutcliffe A (2013) Maternal prepregnancy BMI and child cognition: a longitudinal cohort study. Pediatrics 131(1):56–63. https://doi.org/10.1542/peds.2012-0788
Karras S, Paschou SA, Kandaraki E, Anagnostis P, Annweiler C, Tarlatzis BC, Hollis BW, Grant WB, Goulis DG (2016) Hypovitaminosis D in pregnancy in the Mediterranean region: a systematic review. Eur J Clin Nutr 70(9):979–986. https://doi.org/10.1038/ejcn.2016.12
Deeny SR, van Kleef E, Bou-Antoun S, Hope RJ, Robotham JV (2015) Seasonal changes in the incidence of Escherichia coli bloodstream infection: variation with region and place of onset. Clin Microbiol Infect 21(10):924–929. https://doi.org/10.1016/j.cmi.2015.06.023
Cordeiro CN, Tsimis M, Burd I (2015) Infections and brain development. Obstet Gynecol Surv 70(10):644–655. https://doi.org/10.1097/ogx.0000000000000236
Lips P, van Schoor NM, de Jongh RT (2014) Diet, sun, and lifestyle as determinants of vitamin D status. Ann N Y Acad Sci 1317:92–98. https://doi.org/10.1111/nyas.12443
Garmendia ML, Corvalan C, Uauy R (2014) Assessing the public health impact of developmental origins of health and disease (DOHaD) nutrition interventions. Ann Nutr Metab 64(3–4):226–230. https://doi.org/10.1159/000365024
Livingston LA, Happé F (2017) Conceptualising compensation in neurodevelopmental disorders: reflections from autism spectrum disorder. Neurosci Biobehav Rev 80:729–742. https://doi.org/10.1016/j.neubiorev.2017.06.005
Ajami M, Abdollahi M, Salehi F, Oldewage-Theron W, Jamshidi-Naeini Y (2018) The association between household socioeconomic status, breastfeeding, and infants’ anthropometric indices. Int J Prev Med 9:89. https://doi.org/10.4103/ijpvm.IJPVM_52_17
Brown LJ, Sear R (2017) Local environmental quality positively predicts breastfeeding in the UK’s millennium cohort study. Evol Med Public Health 1:120–135. https://doi.org/10.1093/emph/eox011
Hidaka BH, Kerling EH, Thodosoff JM, Sullivan DK, Colombo J, Carlson SE (2016) Dietary patterns of early childhood and maternal socioeconomic status in a unique prospective sample from a randomized controlled trial of prenatal DHA supplementation. BMC Pediatr 16(1):191. https://doi.org/10.1186/s12887-016-0729-0
McGrath JJ, Eyles DW, Pedersen CB et al (2010) Neonatal vitamin d status and risk of schizophrenia: a population-based case–control study. Arch Gen Psychiatry 67(9):889–894. https://doi.org/10.1001/archgenpsychiatry.2010.110
Holick MF (2007) Vitamin D deficiency. N Engl J Med 357(3):266–281. https://doi.org/10.1056/NEJMra070553
Jones KS, Assar S, Prentice A, Schoenmakers I (2016) Vitamin D expenditure is not altered in pregnancy and lactation despite changes in vitamin D metabolite concentrations. Sci Rep 6:26795. https://doi.org/10.1038/srep26795
Eyles DW, Morley R, Anderson C, Ko P, Burne T, Permezel M, Mortensen PB, Norgaard-Pedersen B, Hougaard DM, McGrath JJ (2010) The utility of neonatal dried blood spots for the assessment of neonatal vitamin D status. Paediatr Perinat Epidemiol 24(3):303–308. https://doi.org/10.1111/j.1365-3016.2010.01105.x
Teasdale TW, Hartmann PV, Pedersen CH, Bertelsen M (2011) The reliability and validity of the Danish Draft Board Cognitive Ability Test: Borge Prien’s Prove. Scand J Psychol 52(2):126–130. https://doi.org/10.1111/j.1467-9450.2010.00862.x
Acknowledgements
The present study was funded by the Programme Commission on Health, Food and Welfare under the Danish Council for Strategic research (Grant number 0603-00453B). We are further grateful to the Oak Foundation for the essential co-financing of the Parker Institute. The funder had no role in data collection and analysis, decision to publish or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All relevant registries are accessible and the collection of data from these registries is in accordance with accepted ethical principles for informed consent according to the Declaration of Helsinki. Statistics Denmark created the relevant sub-data sets anonymized. Permissions from the Danish Data Protection (J. no. 2012-41-1156) and the Ethical Committee of the Capital Region of Denmark (H-3-2011-126) have been granted.
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Specht, I.O., Janbek, J., Thorsteinsdottir, F. et al. Neonatal vitamin D levels and cognitive ability in young adulthood. Eur J Nutr 59, 1919–1928 (2020). https://doi.org/10.1007/s00394-019-02042-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-019-02042-0