Abstract
Purpose
The recurrence of T1 colorectal cancers is relatively rare, and the prognostic factors still remain obscure. This study aimed to clarify the risk factors for recurrence in patients with T1 colorectal cancers treated by endoscopic resection (ER) alone or surgical resection (SR) with lymph node dissection, respectively.
Methods
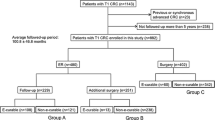
We reviewed 930 patients with resected T1 colorectal cancers (mean follow-up, 52.3 months). Patients were divided into two groups: those who underwent ER alone (298 cases), and those who underwent initial or additional SR with lymph node dissection (632 cases). Group differences in recurrence-free survival were evaluated using the Kaplan–Meier method and log-rank test. Associations between recurrence and clinicopathological features were evaluated in Cox regression analyses; hazard ratios (HRs) were calculated for the total population and each group.
Results
Recurrence occurred in four cases (1.34%) in the ER group and six cases (0.95%) in the SR group (p = 0.32). Endoscopic resection, rectal location, and poor or mucinous (Por/Muc) differentiation were prognostic factors for recurrence in the total population. Por/Muc differentiation was prognostic factor in both groups. Female sex, depressed-type morphology, and lymphatic invasion were also prognostic factors in the ER group, but not in the SR group.
Conclusions
Endoscopic resection, rectal location, and Por/Muc differentiation are prognostic factors in the total population. For patients who undergo ER alone, female sex, depressed-type morphology, and lymphatic invasion are also risk factors for recurrence. For such patients, regional en-bloc surgery with lymph node dissection could reduce the risk of recurrence.



Similar content being viewed by others
References
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ (2009) Cancer statistics, 2009. CA Cancer J Clin 59(4):225–249. https://doi.org/10.3322/caac.20006
Matsuda T, Marugame T, Kamo K, Katanoda K, Ajiki W, Sobue T (2012) Cancer incidence and incidence rates in Japan in 2006: based on data from 15 population-based cancer registries in the monitoring of cancer incidence in Japan (MCIJ) project. Jpn J Clin Oncol 42(2):139–147. https://doi.org/10.1093/jjco/hyr184
Beaton C, Twine CP, Williams GL, Radcliffe AG (2013) Systematic review and meta-analysis of histopathological factors influencing the risk of lymph node metastasis in early colorectal cancer. Colorectal disease: the official journal of the Association of Coloproctology of Great Britain and Ireland 15(7):788–797. https://doi.org/10.1111/codi.12129
Kobayashi N, Saito Y, Uraoka T, Matsuda T, Suzuki H, Fujii T (2009) Treatment strategy for laterally spreading tumors in Japan: before and after the introduction of endoscopic submucosal dissection. J Gastroenterol Hepatol 24(8):1387–1392. https://doi.org/10.1111/j.1440-1746.2009.05893.x
Kyzer S, Begin LR, Gordon PH, Mitmaker B (1992) The care of patients with colorectal polyps that contain invasive adenocarcinoma. Endoscopic polypectomy or colectomy? Cancer 70(8):2044–2050
Tanaka S, Asayama N, Shigita K, Hayashi N, Oka S, Chayama K (2015) Towards safer and appropriate application of endoscopic submucosal dissection for T1 colorectal carcinoma as total excisional biopsy: future perspectives. Digestive endoscopy: official journal of the Japan Gastroenterological Endoscopy Society 27(2):216–222. https://doi.org/10.1111/den.12326
Miyachi H, Kudo SE, Ichimasa K, Hisayuki T, Oikawa H, Matsudaira S, Kouyama Y, Kimura YJ, Misawa M, Mori Y, Ogata N, Kudo T, Kodama K, Hayashi T, Wakamura K, Katagiri A, Baba T, Hidaka E, Ishida F, Kohashi K, Hamatani S (2016) Management of T1 colorectal cancers after endoscopic treatment based on the risk stratification of lymph node metastasis. J Gastroenterol Hepatol 31(6):1126–1132. https://doi.org/10.1111/jgh.13257
Choi DH, Sohn DK, Chang HJ, Lim SB, Choi HS, Jeong SY (2009) Indications for subsequent surgery after endoscopic resection of submucosally invasive colorectal carcinomas: a prospective cohort study. Dis Colon rectum 52(3):438–445. https://doi.org/10.1007/DCR.0b013e318197e37f
Belderbos TD, van Erning FN, de Hingh IH, van Oijen MG, Lemmens VE, Siersema PD (2017) Long-term recurrence-free survival after standard endoscopic resection versus surgical resection of submucosal invasive colorectal cancer: a population-based study. Clin Gastroenterol Hepatol: Off Clin Prac J Am Gastroenterol Assoc 15(3):403–411.e401. https://doi.org/10.1016/j.cgh.2016.08.041
Ikematsu H, Yoda Y, Matsuda T, Yamaguchi Y, Hotta K, Kobayashi N, Fujii T, Oono Y, Sakamoto T, Nakajima T, Takao M, Shinohara T, Murakami Y, Fujimori T, Kaneko K, Saito Y (2013) Long-term outcomes after resection for submucosal invasive colorectal cancers. Gastroenterology 144(3):551–559; quiz e514. https://doi.org/10.1053/j.gastro.2012.12.003
Kobayashi H, Mochizuki H, Morita T, Kotake K, Teramoto T, Kameoka S, Saito Y, Takahashi K, Hase K, Oya M, Maeda K, Hirai T, Kameyama M, Shirouzu K, Sugihara K (2011) Characteristics of recurrence after curative resection for T1 colorectal cancer: Japanese multicenter study. J Gastroenterol 46(2):203–211. https://doi.org/10.1007/s00535-010-0341-2
Boenicke L, Fein M, Sailer M, Isbert C, Germer CT, Thalheimer A (2010) The concurrence of histologically positive resection margins and sessile morphology is an important risk factor for lymph node metastasis after complete endoscopic removal of malignant colorectal polyps. Int J Color Dis 25(4):433–438. https://doi.org/10.1007/s00384-009-0836-6
Kouyama Y, Kudo SE, Miyachi H, Ichimasa K, Hisayuki T, Oikawa H, Matsudaira S, Kimura YJ, Misawa M, Mori Y, Kodama K, Kudo T, Hayashi T, Wakamura K, Katagiri A, Hidaka E, Ishida F, Hamatani S (2016) Practical problems of measuring depth of submucosal invasion in T1 colorectal carcinomas. Int J Color Dis 31(1):137–146. https://doi.org/10.1007/s00384-015-2403-7
Watanabe T, Muro K, Ajioka Y, Hashiguchi Y, Ito Y, Saito Y, Hamaguchi T, Ishida H, Ishiguro M, Ishihara S, Kanemitsu Y, Kawano H, Kinugasa Y, Kokudo N, Murofushi K, Nakajima T, Oka S, Sakai Y, Tsuji A, Uehara K, Ueno H, Yamazaki K, Yoshida M, Yoshino T, Boku N, Fujimori T, Itabashi M, Koinuma N, Morita T, Nishimura G, Sakata Y, Shimada Y, Takahashi K, Tanaka S, Tsuruta O, Yamaguchi T, Yamaguchi N, Tanaka T, Kotake K, Sugihara K (2017) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2016 for the treatment of colorectal cancer. Int J Clin Oncol 23:1–34. https://doi.org/10.1007/s10147-017-1101-6
Schmoll HJ, Van Cutsem E, Stein A, Valentini V, Glimelius B, Haustermans K, Nordlinger B, van de Velde CJ, Balmana J, Regula J, Nagtegaal ID, Beets-Tan RG, Arnold D, Ciardiello F, Hoff P, Kerr D, Kohne CH, Labianca R, Price T, Scheithauer W, Sobrero A, Tabernero J, Aderka D, Barroso S, Bodoky G, Douillard JY, El Ghazaly H, Gallardo J, Garin A, Glynne-Jones R, Jordan K, Meshcheryakov A, Papamichail D, Pfeiffer P, Souglakos I, Turhal S, Cervantes A (2012) ESMO consensus guidelines for management of patients with colon and rectal cancer. A personalized approach to clinical decision making. Ann Oncol: Off J Eur Soc Med Oncol / ESMO 23(10):2479–2516. https://doi.org/10.1093/annonc/mds236
Benson AB 3rd, Venook AP, Cederquist L, Chan E, Chen YJ, Cooper HS, Deming D, Engstrom PF, Enzinger PC, Fichera A, Grem JL, Grothey A, Hochster HS, Hoffe S, Hunt S, Kamel A, Kirilcuk N, Krishnamurthi S, Messersmith WA, Mulcahy MF, Murphy JD, Nurkin S, Saltz L, Sharma S, Shibata D, Skibber JM, Sofocleous CT, Stoffel EM, Stotsky-Himelfarb E, Willett CG, Wu CS, Gregory KM, Freedman-Cass D (2017) Colon cancer, version 1.2017, NCCN clinical practice guidelines in oncology. J Nat Comp Cancer Net: JNCCN 15(3):370–398
Benson AB 3rd, Venook AP, Bekaii-Saab T, Chan E, Chen YJ, Cooper HS, Engstrom PF, Enzinger PC, Fenton MJ, Fuchs CS, Grem JL, Grothey A, Hochster HS, Hunt S, Kamel A, Kirilcuk N, Leong LA, Lin E, Messersmith WA, Mulcahy MF, Murphy JD, Nurkin S, Rohren E, Ryan DP, Saltz L, Sharma S, Shibata D, Skibber JM, Sofocleous CT, Stoffel EM, Stotsky-Himelfarb E, Willett CG, Gregory KM, Freedman-Cass D (2015) Rectal cancer, version 2.2015. J Nat Comp Cancer Net: JNCCN 13(6):719–728 quiz 728
Tamaru Y, Oka S, Tanaka S, Nagata S, Hiraga Y, Kuwai T, Furudoi A, Tamura T, Kunihiro M, Okanobu H, Nakadoi K, Kanao H, Higashiyama M, Arihiro K, Kuraoka K, Shimamoto F, Chayama K (2017) Long-term outcomes after treatment for T1 colorectal carcinoma: a multicenter retrospective cohort study of Hiroshima GI endoscopy research group. J Gastroenterol 52:1169–1179. https://doi.org/10.1007/s00535-017-1318-1
Oka S, Tanaka S, Kanao H, Ishikawa H, Watanabe T, Igarashi M, Saito Y, Ikematsu H, Kobayashi K, Inoue Y, Yahagi N, Tsuda S, Simizu S, Iishi H, Yamano H, Kudo SE, Tsuruta O, Tamura S, Saito Y, Cho E, Fujii T, Sano Y, Nakamura H, Sugihara K, Muto T (2011) Mid-term prognosis after endoscopic resection for submucosal colorectal carcinoma: summary of a multicenter questionnaire survey conducted by the colorectal endoscopic resection standardization implementation working group in Japanese Society for Cancer of the Colon and Rectum. Dig. Endosc: Off J Jpn Gastroenterol Endosc Soc 23(2):190–194. https://doi.org/10.1111/j.1443-1661.2010.01072.x
Nam MJ, Han KS, Kim BC, Hong CW, Sohn DK, Chang HJ, Kim MJ, Kim SY, Baek JY, Park SC, Oh JH (2016) Long-term outcomes of locally or radically resected T1 colorectal cancer. Color Dis: Off J Assoc Coloproctol G B Irel 18(9):852–860. https://doi.org/10.1111/codi.13221
Hotta K, Fujii T, Saito Y, Matsuda T (2009) Local recurrence after endoscopic resection of colorectal tumors. Int J Color Dis 24(2):225–230. https://doi.org/10.1007/s00384-008-0596-8
Di Gregorio C, Bonetti LR, de Gaetani C, Pedroni M, Kaleci S, Ponz de Leon M (2014) Clinical outcome of low- and high-risk malignant colorectal polyps: results of a population-based study and meta-analysis of the available literature. Intern Emerg Med 9(2):151–160. https://doi.org/10.1007/s11739-012-0772-2
Netzer P, Forster C, Biral R, Ruchti C, Neuweiler J, Stauffer E, Schonegg R, Maurer C, Husler J, Halter F, Schmassmann A (1998) Risk factor assessment of endoscopically removed malignant colorectal polyps. Gut 43(5):669–674
Park JJ, Cheon JH, Kwon JE, Shin JK, Jeon SM, Bok HJ, Lee JH, Moon CM, Hong SP, Kim TI, Kim H, Kim WH (2011) Clinical outcomes and factors related to resectability and curability of EMR for early colorectal cancer. Gastrointest Endosc 74(6):1337–1346. https://doi.org/10.1016/j.gie.2011.07.069
Yoshii S, Nojima M, Nosho K, Omori S, Kusumi T, Okuda H, Tsukagoshi H, Fujita M, Yamamoto H, Hosokawa M (2014) Factors associated with risk for colorectal cancer recurrence after endoscopic resection of T1 tumors. Clin Gastroenterol Hepatol: Off Clin Prac J Am Gastroenterol Assoc 12(2):292–302.e293. https://doi.org/10.1016/j.cgh.2013.08.008
Kudo S, Kashida H, Tamura T, Kogure E, Imai Y, Yamano H, Hart AR (2000) Colonoscopic diagnosis and management of nonpolypoid early colorectal cancer. World J Surg 24(9):1081–1090
Ichimasa K, Kudo S, Miyachi H, Kouyama Y, Hayashi T, Wakamura K (2017) Comparative clinicopathological characteristics of colon and rectal T1 carcinoma. Oncol Lett 13:805–810. https://doi.org/10.3892/ol.2016.5464
Kudo S, Tamura S, Nakajima T, Yamano H, Kusaka H, Watanabe H (1996) Diagnosis of colorectal tumorous lesions by magnifying endoscopy. Gastrointest Endosc 44(1):8–14
Bosman FT (2010) World Health Organization, International Agency for Research on Cancer. WHO classification of tumours of the digestive system. International Agency for Research on Cancer 134–146
Steele SR, Chang GJ, Hendren S, Weiser M, Irani J, Buie WD, Rafferty JF (2015) Practice guideline for the surveillance of patients after curative treatment of colon and rectal cancer. Dis Colon rectum 58(8):713–725. https://doi.org/10.1097/dcr.0000000000000410
Wada H, Shiozawa M, Sugano N, Morinaga S, Rino Y, Masuda M, Akaike M, Miyagi Y (2013) Lymphatic invasion identified with D2-40 immunostaining as a risk factor of nodal metastasis in T1 colorectal cancer. Int J Clin Oncol 18(6):1025–1031. https://doi.org/10.1007/s10147-012-0490-9
Overwater A, Kessels K, Elias SG, Backes Y, BWM S, TCJ S, HJM P, de Vos Tot Nederveen Cappel WH, van den Blink A, GJA O, van Bergeijk J, Kerkhof M, JMJ G, Groen JN, van Lelyveld N, Ter Borg F, Wolfhagen F, Siersema PD, Lacle MM, LMG M (2018) Endoscopic resection of high-risk T1 colorectal carcinoma prior to surgical resection has no adverse effect on long-term outcomes. Gut 67(2):284–290. https://doi.org/10.1136/gutjnl-2015-310961
Watanabe D, Toyonaga T, Ooi M, Yoshizaki T, Ohara Y, Tanaka S, Kawara F, Ishida T, Morita Y, Umegaki E, Matsuda T, Sumi Y, Nishio M, Yokozaki H, Azuma T (2017) Clinical outcomes of deep invasive submucosal colorectal cancer after ESD. Surg Endosc 32:2123–2130. https://doi.org/10.1007/s00464-017-5910-5
Okamoto Y, Mitomi H, Ichikawa K, Tomita S, Fujimori T, Igarashi Y (2015) Effect of skip lymphovascular invasion on hepatic metastasis in colorectal carcinomas. Int J Clin Oncol 20(4):761–766. https://doi.org/10.1007/s10147-014-0778-z
Ueno H, Mochizuki H, Hashiguchi Y, Ishiguro M, Miyoshi M, Kajiwara Y, Sato T, Shimazaki H, Hase K (2007) Extramural cancer deposits without nodal structure in colorectal cancer: optimal categorization for prognostic staging. Am J Clin Pathol 127(2):287–294. https://doi.org/10.1309/903ut10vq3lc7b8l
Ueno H, Mochizuki H, Hashiguchi Y, Shimazaki H, Aida S, Hase K, Matsukuma S, Kanai T, Kurihara H, Ozawa K, Yoshimura K, Bekku S (2004) Risk factors for an adverse outcome in early invasive colorectal carcinoma. Gastroenterology 127(2):385–394
Kobayashi H, Higuchi T, Uetake H, Iida S, Ishikawa T, Ishiguro M, Sugihara K (2012) Resection with en bloc removal of regional lymph node after endoscopic resection for T1 colorectal cancer. Ann Surg Oncol 19(13):4161–4167. https://doi.org/10.1245/s10434-012-2471-7
Wang HS, Liang WY, Lin TC, Chen WS, Jiang JK, Yang SH, Chang SC, Lin JK (2005) Curative resection of T1 colorectal carcinoma: risk of lymph node metastasis and long-term prognosis. Dis Colon rectum 48(6):1182–1192. https://doi.org/10.1007/s10350-004-0935-y
Kikuchi R, Takano M, Takagi K, Fujimoto N, Nozaki R, Fujiyoshi T, Uchida Y (1995) Management of early invasive colorectal cancer. Risk of recurrence and clinical guidelines. Dis Colon rectum 38(12):1286–1295
Wang H, Wei XZ, Fu CG, Zhao RH, Cao FA (2010) Patterns of lymph node metastasis are different in colon and rectal carcinomas. World J Gastroenterol 16(42):5375–5379
Bosch SL, Teerenstra S, de Wilt JH, Cunningham C, Nagtegaal ID (2013) Predicting lymph node metastasis in pT1 colorectal cancer: a systematic review of risk factors providing rationale for therapy decisions. Endoscopy 45(10):827–834. https://doi.org/10.1055/s-0033-1344238
Ichimasa K, Kudo S, Miyachi H (2016) Patient gender as a factor associated with lymph node metastasis in T1 colorectal cancer: a systematic review and meta-analysis. Mol Clin Oncol 6:517–524. https://doi.org/10.3892/mco.2017.1172
Fujii T, Rembacken BJ, Dixon MF, Yoshida S, Axon AT (1998) Flat adenomas in the United Kingdom: are treatable cancers being missed? Endoscopy 30(5):437–443. https://doi.org/10.1055/s-2007-1001304
Rembacken BJ, Fujii T, Cairns A, Dixon MF, Yoshida S, Chalmers DM, Axon AT (2000) Flat and depressed colonic neoplasms: a prospective study of 1000 colonoscopies in the UK. Lancet (London, England) 355(9211):1211–1214
Tateishi Y, Nakanishi Y, Taniguchi H, Shimoda T, Umemura S (2010) Pathological prognostic factors predicting lymph node metastasis in submucosal invasive (T1) colorectal carcinoma. Modern Pathol : Off J US Can Acad Pathol Inc 23(8):1068–1072. https://doi.org/10.1038/modpathol.2010.88
Acknowledgments
The authors express great thanks to Chiaki Nishimura for helping with the statistical analyses, and to all members of the Digestive Disease Center Showa University Northern Yokohama Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Kouyama, Y., Kudo, Se., Miyachi, H. et al. Risk factors of recurrence in T1 colorectal cancers treated by endoscopic resection alone or surgical resection with lymph node dissection. Int J Colorectal Dis 33, 1029–1038 (2018). https://doi.org/10.1007/s00384-018-3081-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-018-3081-z