Abstract
Objective
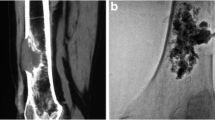
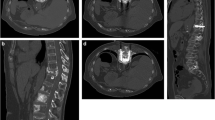
To evaluate low-pressure bone stenting combined with cementoplasty in extensive lytic lesions.
Methods
A single-centre study involving four consecutive patients (four women) with extensive lytic tumours was performed. The average age was 65 years. Surgical treatment was not indicated or not wished for by the patients. Institutional review board approval and informed consent were obtained. Percutaneous consolidation was performed by an interventional radiologist under fluoroscopy guidance. Follow-up was assessed using the visual analogue scale (VAS).
Results
Under general (n = 2) or local (n = 2) anaesthesia, five 11-gauge bone biopsy needles were advanced in four lesions. Five auto-expandable uncovered stents (10-14 mm diameter and 40-60 mm long) were inserted. In all cases, bone cement was successfully placed into the tumours. The volume of cement that was injected through the cannulas into the stents was 5-10 mL. Using VAS, pain decreased from more than 9/10 preoperatively to less than 2/10 after the procedure for all patients (p < 0.05). No complications occurred during the follow-up (8-19 months).
Conclusion
This study suggests that cementoplasty combined with low-pressure bone stenting could allow effective bone stabilization resulting in pain relief.
Key Points
• Low-pressure bone stenting is possible.
• This technique improves cement injection control.
• The procedure allows effective bone stabilization resulting in pain relief.



Similar content being viewed by others
References
Chiras J, Cormier E, Baragan H, Jean B, Rose M (2007) Interventional radiology in bone metastases. Bull Cancer 94(2):161–169
Gangi A, Buy X (2010) Percutaneous bone tumor management. Semin Interv Radiol 27(2):124–136
Deschamps F, de Baere T (2012) Cementoplasty of bone metastases. Diagn Interv Imaging 93(9):685–689
Cazzato RL, Buy X, Eker O, Fabre T, Palussiere J (2014) Percutaneous long bone cementoplasty of the limbs: experience with fifty-one non-surgical patients. Eur Radiol 24(12):3059–3068
Liu XW, Jin P, Liu K et al (2016) Comparison of percutaneous long bone cementoplasty with or without embedding a cement-filled catheter for painful long bone metastases with impending fracture. Eur Radiol
Santiago FR, Del Mar Castellano Garcia M, Montes JL, Garcia MR, Fernandez JM (2009) Treatment of bone tumours by radiofrequency thermal ablation. Curr Rev Muscoskelet Med 2(1):43–50
Deschamps F, Farouil G, de Baere T (2014) Percutaneous ablation of bone tumors. Diagn Interv Imaging 95(7-8):659–663
Carrafiello G, Lagana D, Recaldini C et al (2007) Combined treatment of ablative therapy with percutaneous radiofrequency and cementoplasty of a symptomatic metastatic lesion of the acetabulum. Australas Radiol 51(Suppl):B344–348
Kastler B, Jacamon M, Aubry S et al (2007) Combined bipolar radiofrequency and cementoplasty of bone metastases. J Radiol 88(9 Pt 2):1242–1247
Cruz JP, Sahgal A, Whyne C, Fehlings MG, Smith R (2014) Tumor extravasation following a cement augmentation procedure for vertebral compression fracture in metastatic spinal disease. Journal of neurosurgery. Spine 21(3):372–377
Fourney DR, Schomer DF, Nader R et al (2003) Percutaneous vertebroplasty and kyphoplasty for painful vertebral body fractures in cancer patients. J Neurosurg 98(1 Suppl):21–30
Lee MJ, Dumonski M, Cahill P, Stanley T, Park D, Singh K (2009) Percutaneous treatment of vertebral compression fractures: a meta-analysis of complications. Spine (Phila Pa 1976) 34(11):1228–1232
Deschamps F, Farouil G, Hakime A et al (2012) Cementoplasty of metastases of the proximal femur: is it a safe palliative option? J Vasc Interv Radiol 23(10):1311–1316
Berenson J, Pflugmacher R, Jarzem P et al (2011) Balloon kyphoplasty versus non-surgical fracture management for treatment of painful vertebral body compression fractures in patients with cancer: a multicentre, randomised controlled trial. Lancet Oncol 12(3):225–235
Deschamps F, Farouil G, Hakime A, Teriitehau C, Barah A, de Baere T (2012) Percutaneous stabilization of impending pathological fracture of the proximal femur. Cardiovasc Intervent Radiol 35(6):1428–1432
Heini PF, Teuscher R (2012) Vertebral body stenting / stentoplasty. Swiss Med Wkly 142:w13658
Martin-Lopez JE, Pavon-Gomez MJ, Romero-Tabares A, Molina-Lopez T (2015) Stentoplasty effectiveness and safety for the treatment of osteoporotic vertebral fractures: a systematic review. Orthop Traumatol Surg Res 101(5):627–632
Kaczmarek K, Wiacek MP, Sulewski A, Kubaszewski L, Kaczmarczyk J, Nowakowski A (2014) Failure and success in the treatment of breast carcinoma in men: a case report. Pol Orthop Traumatol 79:1–4
Capel C, Fichten A, Nicot B et al (2014) Should we fear cement leakage during kyphoplasty in percutaneous traumatic spine surgery? A single experience with 76 consecutive cases. Neurochirurgie 60(6):293–298
Lador R, Liberman S, Ben-Galim P, Dreiangel N, Reitman CA, Hipp JA (2013) A cadaver study to compare vertebral augmentation with a high-viscosity cement to augmentation with conventional lower-viscosity cement. J Spinal Disord Tech 26(2):68–73
Georgy BA, Wong W (2007) Plasma-mediated radiofrequency ablation assisted percutaneous cement injection for treating advanced malignant vertebral compression fractures. AJNR Am J Neuroradiol 28(4):700–705
Pusceddu C, Sotgia B, Fele RM, Ballicu N, Melis L (2016) Combined Microwave Ablation and Cementoplasty in Patients with Painful Bone Metastases at High Risk of Fracture. Cardiovasc Intervent Radiol 39(1):74–80
Anselmetti GC, Manca A, Ortega C, Grignani G, Debernardi F, Regge D (2008) Treatment of extraspinal painful bone metastases with percutaneous cementoplasty: a prospective study of 50 patients. Cardiovasc Intervent Radiol 31(18704572):1165–1173
Dayer R, Peter R (2008) Percutaneous cementoplasty complicating the treatment of a pathologic subtrochanteric fracture: a case report. Injury 39(18539281):801–804
Van der Linden YM, Dijkstra PD, Kroon HM et al (2004) Comparative analysis of risk factors for pathological fracture with femoral metastases. J Bone Joint Surg (Br) 86(4):566–573
Dalbayrak S, Onen MR, Yilmaz M, Naderi S (2010) Clinical and radiographic results of balloon kyphoplasty for treatment of vertebral body metastases and multiple myelomas. J Clin Neurosci: Off J Neurosurg Soc Australas 17(2):219–224
Dhir V, Artifon EL, Gupta K et al (2013) Multicenter study on endoscopic ultrasound-guided expandable biliary metal stent placement: choice of access route, direction of stent insertion, and drainage route. Dig Endosc: Off J Jpn Gastroenterol Endosc Soc
Acknowledgements
The scientific guarantor of this publication is Olivier Hauger.
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
The authors state that this work has not received any funding.
No complex statistical methods were necessary for this paper.
Institutional review board approval was obtained.
Written informed consent was obtained from all subjects (patients) in this study.
Methodology:
• prospective
• observational
• performed at one institution
The authors thank Pippa McKelvie-Sebileau for medical editorial services.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cornelis, F.H., Petitpierre, F., Fabre, T. et al. Percutaneous low-pressure bone stenting to control cement deposition in extensive lytic lesions. Eur Radiol 27, 3942–3946 (2017). https://doi.org/10.1007/s00330-016-4703-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-016-4703-x