Abstract
Background
Juvenile idiopathic inflammatory myopathy is a rare yet potentially debilitating condition. MRI is used both for diagnosis and to assess response to treatment. No study has evaluated the performance of US elastography in the diagnosis of this condition in children.
Objective
To assess the performance of compression–strain US elastography in detecting active myositis in children with clinically confirmed juvenile idiopathic inflammatory myopathy and to compare its efficacy to MRI.
Materials and methods
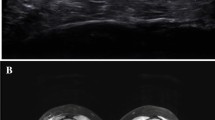
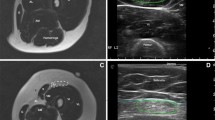
Children with juvenile idiopathic inflammatory myopathy underwent non-contrast MR imaging as well as compression–strain US elastography of the quadriceps muscles. Imaging findings from both modalities were compared to each other as well as to the clinical determination of active disease based on physical examination and laboratory data. Active myositis on MR was defined as increased muscle signal on T2-weighted images. Elastography images were defined as normal or abnormal based on a previously published numerical scale of muscle elastography in normal children. Muscle echogenicity was graded as normal or abnormal based on gray-scale sonographic images.
Results
Twenty-one studies were conducted in 18 pediatric patients (15 female, 3 male; age range 3–19 years). Active myositis was present on MRI in ten cases. There was a significant association between abnormal MRI and clinically active disease (P = 0.012). US elastography was abnormal in 4 of 10 cases with abnormal MRI and in 4 of 11 cases with normal MRI. There was no association between abnormal elastography and either MRI (P > 0.999) or clinically active disease (P > 0.999). Muscle echogenicity was normal in 11 patients; all 11 had normal elastography. Of the ten patients with increased muscle echogenicity, eight had abnormal elastography. There was a significant association between muscle echogenicity and US elastography (P < 0.001). The positive and negative predictive values for elastography in the determination of active myositis were 75% and 31%, respectively, with a sensitivity of 40% and specificity of 67%.
Conclusion
Compression–strain US elastography does not accurately detect active myositis in children with juvenile idiopathic inflammatory myopathy and cannot replace MRI as the imaging standard for detecting myositis in these children. The association between abnormal US elastography and increased muscle echogenicity suggests that elastography is capable of detecting muscle derangement in patients with myositis; however further studies are required to determine the clinical significance of these findings.



Similar content being viewed by others
References
Robinson AB, Reed AM (2011) Juvenile dermatomyositis. In: Kliegman RM, Stanton B, St. Geme J et al (eds) Nelson textbook of pediatrics, 19th edn. Saunders, Philadelphia, pp 846–850
Rider LG, Katz JD, Jones OY (2013) Developments in the classification and treatment of the juvenile idiopathic inflammatory myopathies. Rheum Dis Clin North Am 39:877–904
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (first of two parts). N Engl J Med 292:344–347
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (second of two parts). N Engl J Med 292:403–407
Brown VE, Pilkington CA, Feldman BM et al (2006) An international consensus survey of the diagnostic criteria for juvenile dermatomyositis (JDM). Rheumatology 45:990–993
Hernandez RJ, Keim DR, Sullivan DB et al (1990) Magnetic resonance imaging appearance of the muscles in childhood dermatomyositis. J Pediatr 117:546–550
Hernandez RJ, Sullivan DB, Chenevert TL et al (1993) MR imaging in children with dermatomyositis: musculoskeletal findings and correlation with clinical and laboratory findings. AJR Am J Roentgenol 161:359–366
Garra BS (2007) Imaging and estimation of tissue elasticity by ultrasound. Ultrasound Q 23:255–268
Klauser AS, Peetrons P (2010) Developments in musculoskeletal ultrasound and clinical applications. Skeletal Radiol 39:1061–1071
De Zordo T, Chhem R, Smekal V et al (2010) Real-time sonoelastography: findings in patients with symptomatic Achilles tendons and comparison to healthy volunteers. Ultraschall Med 31:394–400
Tan S, Kudaş S, Özcan AS et al (2012) Real-time sonoelastography of the Achilles tendon: pattern description in healthy subjects and patients with surgically repaired complete ruptures. Skeletal Radiol 41:1067–1072
Sconfienza LM, Silvestri E, Cimmino MA (2010) Sonoelastography in the evaluation of painful Achilles tendon in amateur athletes. Clin Exp Rheumatol 28:373–378
De Zordo T, Fink C, Feuchtner GM et al (2009) Real-time sonoelastography findings in healthy Achilles tendons. AJR Am J Roentgenol 193:W134–138
De Zordo T, Lill SR, Fink C et al (2009) Real-time sonoelastography of lateral epicondylitis: comparison of findings between patients and healthy volunteers. AJR Am J Roentgenol 193:180–185
Berko NS, Fitzgerald EF, Amaral TD et al (2014) Ultrasound elastography in children: establishing the normal range of muscle elasticity. Pediatr Radiol 44:158–163
Kwon DR, Park GY, Lee SU et al (2012) Spastic cerebral palsy in children: dynamic sonoelastographic findings of medial gastrocnemius. Radiology 263:794–801
Vasilescu D, Vasilescu D, Dudea S et al (2010) Sonoelastography contribution in cerebral palsy spasticity treatment assessment, preliminary report: a systematic review of the literature apropos of seven patients. Med Ultrason 12:306–310
Wedderburn LR, Varsani H, Li CK et al (2007) International consensus on a proposed score system for muscle biopsy evaluation in patients with juvenile dermatomyositis: a tool for potential use in clinical trials. Arthritis Rheum 57:1192–1201
Lovell DJ, Lindsley CB, Rennebohm RM et al (1999) Development of validated disease activity and damage indices for the juvenile idiopathic inflammatory myopathies. II. The childhood myositis assessment scale (CMAS): a quantitative tool for the evaluation of muscle function. The juvenile dermatomyositis disease activity collaborative study group. Arthritis Rheum 42:2213–2219
Lazarevic D, Pistorio A, Palmisani E et al (2013) The PRINTO criteria for clinically inactive disease in juvenile dermatomyositis. Ann Rheum Dis 72:686–693
Felson DT, Anderson JJ, Boers M et al (1995) American college of rheumatology. Preliminary definition of improvement in rheumatoid arthritis. Arthritis Rheum 38:727–735
Rider LG, Feldman BM, Perez MD et al (1997) Development of validated disease activity and damage indices for the juvenile idiopathic inflammatory myopathies: I. Physician, parent, and patient global assessments. Juvenile dermatomyositis disease activity collaborative study group. Arthritis Rheum 40:1976–1983
Tomasová Studynková J, Charvát F, Jarosová K et al (2007) The role of MRI in the assessment of polymyositis and dermatomyositis. Rheumatology 46:1174–1179
Fraser DD, Frank JA, Dalakas M et al (1991) Magnetic resonance imaging in the idiopathic inflammatory myopathies. J Rheumatol 18:1693–1700
Botar-Jid C, Damian L, Dudea SM et al (2010) The contribution of ultrasonography and sonoelastography in assessment of myositis. Med Ultrason 12:120–126
Tansley SL, McHugh NJ, Wedderburn LR (2013) Adult and juvenile dermatomyositis: are the distinct clinical features explained by our current understanding of serological subgroups and pathogenic mechanisms? Arthritis Res Ther 8:211
Zamorani MP, Valle M (2007) Muscle and tendon. In: Bianchi S, Martinoli C (eds) Ultrasound of the musculoskeletal system. Springer, Berlin Heidelberg, pp 45–96
Hu CF, Chen CP, Tsai WC et al (2012) Quantification of skeletal muscle fibrosis at different healing stages using sonography: a morphologic and histologic study in an animal model. J Ultrasound Med 31:43–48
Reimers K, Reimers CD, Wagner S et al (1993) Skeletal muscle sonography: a correlative study of echogenicity and morphology. J Ultrasound Med 12:73–77
McCullough MB, Domire ZJ, Reed AM et al (2011) Evaluation of muscles affected by myositis using magnetic resonance elastography. Muscle Nerve 43:585–590
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Berko, N.S., Hay, A., Sterba, Y. et al. Efficacy of ultrasound elastography in detecting active myositis in children: can it replace MRI?. Pediatr Radiol 45, 1522–1528 (2015). https://doi.org/10.1007/s00247-015-3350-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-015-3350-8