Abstract
Introduction and hypothesis
The relationship between pelvic floor muscles and measurements of urethral function is not well studied. It is not known whether adjusting for clinical, demographic and urodynamic parameters would improve the association between MUCP and ALPP. Our hypothesis was that pelvic floor muscle strength (PFMS) influences the relationship between MUCP and ALPP.
Methods
This was a retrospective study of women who underwent a complex urodynamic study with evaluation of MUCP and ALPP using ICD-9 codes with documentation of PFMS.
Results
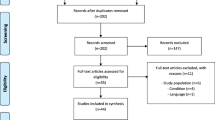
Urodynamic stress incontinence was confirmed in 478 patients, of whom 323 had MUCP recorded and 263 had both MUCP and ALPP recorded. Women with higher PFMS had a higher MUCP. In regression analysis ALPP at 150 mL and MUCP were weakly associated (coefficient 0.43, 95% CI 0.08–0.78; p = 0.02), whereas ALPP at capacity and MUCP were moderately associated (coefficient 0.60, 95% CI 0.25–0.95; p < 0.001).
Conclusions
This study showed that MUCP and ALPP at 150 mL were weakly associated and that this improved to a moderate association for ALPP at capacity. MUCP increased with increasing PFMS among women with stress urinary incontinence and decreased with increasing age. There was no evidence that ALPP was associated with PFMS or age. The relationship between MUCP and ALPP was unchanged when accounting for covariates of PFMS (age, parity, BMI, prior procedure, urethral mobility, bladder capacity, stage of cystocele, or stage of uterine or apical prolapse).

Similar content being viewed by others
References
Ebbesen MH, Hunskaar S, Rortveit G, Hannestad YS. Prevalence, incidence and remission of urinary incontinence in women: longitudinal data from the Norwegian HUNT study (EPINCONT). BMC Urol. 2013;13:27. doi:10.1186/1471-2490-13-27.
Ko Y, Lin SJ, Salmon JW, Bron MS. The impact of urinary incontinence on quality of life of the elderly. Am J Manag Care. 2005;11(4 Suppl):S103–11.
Abrams P, Andersson KE, Birder L, et al. Fourth International Consultation on Incontinence Recommendations of the International Scientific Committee: Evaluation and treatment of urinary incontinence, pelvic organ prolapse, and fecal incontinence. Neurourol Urodyn. 2010;29(1):213–40. doi:10.1002/nau.20870.
Haylen BT, de Ridder D, Freeman RM, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21(1):5–26. doi:10.1007/s00192-009-0976-9.
Sultana CJ. Urethral closure pressure and leak-point pressure in incontinent women. Obstet Gynecol. 1995;86(5):839–42.
Swift SE, Ostergard DR. A comparison of stress leak-point pressure and maximal urethral closure pressure in patients with genuine stress incontinence. Obstet Gynecol. 1995;85(5 Pt 1):704–8.
Nager CW, Schulz JA, Stanton SL, Monga A. Correlation of urethral closure pressure, leak-point pressure and incontinence severity measures. Int Urogynecol J. 2001;12(6):395–400. doi:10.1007/s001920170020.
White T, Kawasaki A, Ross RV, Adam RA, Duong TH. Correlation of maximum urethral closure pressure with Valsalva leak point pressure using air-charged urodynamic catheters. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20(9):1109–12. doi:10.1007/s00192-009-0910-1.
Feldner Jr PC, Bezerra LR, de Castro RA, et al. Correlation between Valsalva leak point pressure and maximal urethral closure pressure in women with stress urinary incontinence. Int Urogynecol J. 2004;15(3):194–7. doi:10.1007/s00192-004-1130-3.
Murphy M, Culligan PJ, Graham CA, Kubik KM, Heit MH. Is the leak point pressure alone an accurate indicator of intrinsic sphincteric deficiency? Int Urogynecol J. 2004;15(5):294–7. doi:10.1007/s00192-004-1154-8.
Chai TC, Huang L, Kenton K, et al. Association of baseline urodynamic measures of urethral function with clinical, demographic, and other urodynamic variables in women prior to undergoing midurethral sling surgery. Neurourol Urodyn. 2012;31(4):496–501. doi:10.1002/nau.21198.
Baessler K, Miska K, Draths R, Schuessler B. Effects of voluntary pelvic floor contraction and relaxation on the urethral closure pressure. Int Urogynecol J Pelvic Floor Dysfunct. 2005;16(3):187–90. discussion 190–1 doi:10.1007/s00192-004-1232-y.
Lemack GE, Xu Y, Brubaker L, et al. Clinical and demographic factors associated with Valsalva leak point pressure among women undergoing Burch bladder neck suspension or autologous rectus fascial sling procedures. Neurourol Urodyn. 2007;26(3):392–6. doi:10.1002/nau.20325.
Zubieta M, Carr RL, Drake MJ, Bø K. Influence of voluntary pelvic floor muscle contraction and pelvic floor muscle training on urethral closure pressures: a systematic literature review. Int Urogynecol J. 2016;27(5):687–96. doi:10.1007/s00192-015-2856-9.
Benvenuti F, Caputo GM, Bandinelli S, Mayer F, Biagini C, Sommavilla A. Reeducative treatment of female genuine stress incontinence. Am J Phys Med. 1987;66(4):155–68.
Bump RC, Mattiasson A, Bø K, et al. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol. 1996;175(1):10–7.
Bø K, Finckenhagen HB. Vaginal palpation of pelvic floor muscle strength: inter-test reproducibility and comparison between palpation and vaginal squeeze pressure. Acta Obstet Gynecol Scand. 2001;80(10):883–7.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap) – a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–81. doi:10.1016/j.jbi.2008.08.010.
Kenton K, Brubaker L. Relationship between levator ani contraction and motor unit activation in the urethral sphincter. Am J Obstet Gynecol. 2002;187(2):403–6.
Bremer RE, Barber MD, Coates KW. Innervation of the levator ani and coccygeus muscles of the female rat. Anat Rec A Discov Mol Cell Evol Biol. 2003;275(1):1031–41.
Henneman E, Clamann HP, Gillies JD. Rank order of motoneurons within a pool: law of combination. J Neurophysiol. 1974;37(6):1338–49.
Obrink A, Bunne G, Ulmsten U. Intra-urethral and intra-vesical pressure in continent women. Acta Obstet Gynecol Scand. 1977;56(5):525–9.
Rud T. Urethral pressure profile in continent women from childhood to old age. Acta Obstet Gynecol Scand. 1980;59(4):331–5.
Pfisterer MH, Griffiths DJ, Schaefer PW, Resnick NM. The effect of age on lower urinary tract function: a study in women. J Am Geriatr Soc. 2006;54(3):405–12. doi:10.1111/j.1532-5415.2005.00613.x.
Pandit M, DeLancey JO, Ashton-Miller JA, Iyengar J, Blaivas M, Perucchini D. Quantification of intramuscular nerves within the female striated urogenital sphincter muscle. Obstet Gynecol. 2000;95(6 Pt 1):797–800.
van Loenen NT, Vierhout ME. Augmentation of urethral pressure profile by voluntary pelvic floor contraction. Int Urogynecol J. 1997;8(5):284–7. doi:10.1007/BF02765485.
Teleman PM, Mattiasson A. Urethral pressure response patterns induced by squeeze in continent and incontinent women. Int Urogynecol J Pelvic Floor Dysfunct. 2007;18(9):1027–31. doi:10.1007/s00192-006-0284-6.
Neumann PB, Grimmer KA, Deenadayalan Y. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. BMC Womens Health. 2006;6:11. doi:10.1186/1472-6874-6-11.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The Vanderbilt University Medical Center’s Synthetic Derivative is supported by institutional funding and by the CTSA grant ULTR000445 from NCATS/NIH.
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Hill, B.J., Fletcher, S., Blume, J. et al. Variables affecting maximum urethral closure pressure (MUCP) and abdominal leak point pressure (ALPP) measurements. Int Urogynecol J 28, 1651–1656 (2017). https://doi.org/10.1007/s00192-017-3331-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-017-3331-6