Abstract
Purpose
The endothelial protein C receptor (EPCR) negatively regulates the coagulopathy and inflammatory response in sepsis. Mechanisms controlling the expression of cell-bound and circulating soluble EPCR (sEPCR) are still unclear. Moreover, the clinical impact of EPCR shedding and its potential value to predict sepsis progression and outcome remain to be established.
Methods
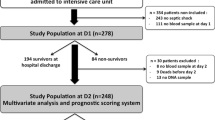
We investigated the time course of plasma sEPCR over the 5 first days (D) of severe sepsis in 40 patients.
Results
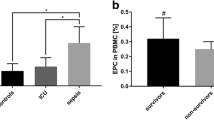
No significant difference was observed when comparing sEPCR at admission (D1) to healthy volunteers and to patients with vasculitis. We report that the kinetics profile of plasma sEPCR in patients was almost stable at the onset of sepsis with no change from D1 to D4 and then a significant decrease at D5. This pattern of release was consistently observed whatever the level of sEPCR at D1. Characteristics of patients or of infections (except Gram negative) had no or little critical influence on the sEPCR profile. However, we found that sEPCR kinetics was clearly associated with patient’s outcome (D28 survival). We demonstrate that a significant but moderate (<15% of basal level) and transient increase in sEPCR level at D2 is associated with poor outcome at D28.
Conclusion
Severe sepsis, at the onset, only triggers moderate quantitative changes in plasma sEPCR levels. Our findings suggest that in severe sepsis, an early (at D2), transient but significant increase in circulating sEPCR may be detrimental suggesting that sEPCR could provide an early biological marker of sepsis outcome.


Similar content being viewed by others
Abbreviations
- APC:
-
Activated protein C
- EC:
-
Endothelial cell
- EPCR:
-
Endothelial protein C receptor
- ICU:
-
Intensive care unit
- MPA:
-
Microscopic polyangiitis
- PC:
-
Protein C
- SAPS:
-
Simplified Acute Physiology Score
- mEPCR:
-
Membrane EPCR
- sEPCR:
-
Soluble EPCR
- SIRS:
-
Systemic inflammatory response syndrome
- SOFA:
-
Sepsis-related Organ Failure Assessment
- TF:
-
Tissue factor
- TM:
-
Thrombomodulin
- TNFα:
-
Tumor necrosis factor-alpha
- WG:
-
Wegener granulomatosis
References
Esmon CT (2002) Protein C pathway in sepsis. Ann Med 34:598–605
Mackman N (2004) Role of tissue factor in hemostasis, thrombosis, and vascular development. Arterioscler Thromb Vasc Biol 24:1015–1022
Fukudome K, Esmon CT (1994) Identification, cloning, and regulation of a novel endothelial cell protein C/activated protein C receptor. J Biol Chem 269:26486–26491
Joyce DE, Gelbert L, Ciaccia A, DeHoff B, Grinnell BW (2001) Gene expression profile of antithrombotic protein c defines new mechanisms modulating inflammation and apoptosis. J Biol Chem 276:11199–11203
Riewald M, Petrovan RJ, Donner A, Mueller BM, Ruf W (2002) Activation of endothelial cell protease activated receptor 1 by the protein C pathway. Science 296:1880–1882
Feistritzer C, Schuepbach RA, Mosnier LO, Bush LA, Di Cera E, Griffin JH, Riewald M (2006) Protective signaling by activated protein C is mechanistically linked to protein C activation on endothelial cells. J Biol Chem 281:20077–20084
Isermann B, Vinnikov IA, Madhusudhan T, Herzog S, Kashif M, Blautzik J, Corat MA, Zeier M, Blessing E, Oh J, Gerlitz B, Berg DT, Grinnell BW, Chavakis T, Esmon CT, Weiler H, Bierhaus A, Nawroth PP (2007) Activated protein C protects against diabetic nephropathy by inhibiting endothelial and podocyte apoptosis. Nat Med 13:1349–1358
Ghosh S, Pendurthi UR, Steinoe A, Esmon CT, Rao LV (2007) Endothelial cell protein C receptor acts as a cellular receptor for factor VIIa on endothelium. J Biol Chem 282:11849–11857
Lopez-Sagaseta J, Montes R, Puy C, Diez N, Fukudome K, Hermida J (2007) Binding of factor VIIa to the endothelial cell protein C receptor reduces its coagulant activity. J Thromb Haemost 5:1817–1824
Laszik Z, Mitro A, Taylor FB Jr, Ferrell G, Esmon CT (1997) Human protein C receptor is present primarily on endothelium of large blood vessels: implications for the control of the protein C pathway. Circulation 96:3633–3640
Gu JM, Crawley JT, Ferrell G, Zhang F, Li W, Esmon NL, Esmon CT (2002) Disruption of the endothelial cell protein C receptor gene in mice causes placental thrombosis and early embryonic lethality. J Biol Chem 277:43335–43343
Kurosawa S, Stearns-Kurosawa DJ, Carson CW, D’Angelo A, Della Valle P, Esmon CT (1998) Plasma levels of endothelial cell protein C receptor are elevated in patients with sepsis and systemic lupus erythematosus: lack of correlation with thrombomodulin suggests involvement of different pathological processes. Blood 91:725–727
Xu J, Qu D, Esmon NL, Esmon CT (2000) Metalloproteolytic release of endothelial cell protein C receptor. J Biol Chem 275:6038–6044
Qu D, Wang Y, Esmon NL, Esmon CT (2007) Regulated endothelial protein C receptor shedding is mediated by tumor necrosis factor-alpha converting enzyme/ADAM17. J Thromb Haemost 5:395–402
Saposnik B, Lesteven E, Lokajczyk A, Esmon CT, Aiach M, Gandrille S (2008) Alternative mRNA is favored by the A3 haplotype of the EPCR gene PROCR and generates a novel soluble form of EPCR in plasma. Blood 111:3442–3451
Liaw PC, Neuenschwander PF, Smirnov MD, Esmon CT (2000) Mechanisms by which soluble endothelial cell protein C receptor modulates protein C and activated protein C function. J Biol Chem 275:5447–5452
Esmon CT (2006) The endothelial protein C receptor. Curr Opin Hematol 13:382–385
Saposnik B, Reny JL, Gaussem P, Emmerich J, Aiach M, Gandrille S (2004) A haplotype of the EPCR gene is associated with increased plasma levels of sEPCR and is a candidate risk factor for thrombosis. Blood 103:1311–1318
Simioni P, Morboeuf O, Tognin G, Gavasso S, Tormene D, Woodhams B, Pagnan A (2006) Soluble endothelial protein C receptor (sEPCR) levels and venous thromboembolism in carriers of two dysfunctional protein C variants. Thromb Res 117:523–528
American College of Chest Physicians/Society of Critical Care Medicine (1992) American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med 20:864-874
Coupel S, Moreau A, Hamidou M, Horejsi V, Soulillou JP, Charreau B (2007) Expression and release of soluble HLA-E is an immunoregulatory feature of endothelial cell activation. Blood 109:2806–2814
Esmon CT (2003) Coagulation and inflammation. J Endotoxin Res 9:192–198
Aird WC (2003) The role of the endothelium in severe sepsis and multiple organ dysfunction syndrome. Blood 101:3765–3777
Taylor FB Jr, Stearns-Kurosawa DJ, Kurosawa S, Ferrell G, Chang AC, Laszik Z, Kosanke S, Peer G, Esmon CT (2000) The endothelial cell protein C receptor aids in host defense against Escherichia coli sepsis. Blood 95:1680–1686
Taylor FB Jr, Peer GT, Lockhart MS, Ferrell G, Esmon CT (2001) Endothelial cell protein C receptor plays an important role in protein C activation in vivo. Blood 97:1685–1688
Liaw PC, Esmon CT, Kahnamoui K, Schmidt S, Kahnamoui S, Ferrell G, Beaudin S, Julian JA, Weitz JI, Crowther M, Loeb M, Cook D (2004) Patients with severe sepsis vary markedly in their ability to generate activated protein C. Blood 104:3958–3964
Faust SN, Levin M, Harrison OB, Goldin RD, Lockhart MS, Kondaveeti S, Laszik Z, Esmon CT, Heyderman RS (2001) Dysfunction of endothelial protein C activation in severe meningococcal sepsis. N Engl J Med 345:408–416
Borgel D, Bornstain C, Reitsma PH, Lerolle N, Gandrille S, Dali-Ali F, Esmon CT, Fagon JY, Aiach M, Diehl JL (2007) A comparative study of the protein C pathway in septic and nonseptic patients with organ failure. Am J Respir Crit Care Med 176:878–885
Guitton C, Gérard N, Quillard T, Charreau B (2011) Circulating endothelial cell protein C receptor: endothelial regulation and cumulative impact of gender and A3 haplotype. J Vasc Res 48:336–346. doi:101159/000322582
Fine MJ, Smith MA, Carson CA, Mutha SS, Sankey SS, Weissfeld LA, Kapoor WN (1996) Prognosis and outcomes of patients with community-acquired pneumonia. A meta-analysis. JAMA 275:134–141
Eachempati SR, Hydo L, Barie PS (1999) Gender-based differences in outcome in patients with sepsis. Arch Surg 134:1342–1347
Adrie C, Azoulay E, Francais A, Clec’h C, Darques L, Schwebel C, Nakache D, Jamali S, Goldgran-Toledano D, Garrouste-Orgeas M, Timsit JF (2007) Influence of gender on the outcome of severe sepsis: a reappraisal. Chest 132:1786–1793
Bernard GR, Vincent JL, Laterre PF, LaRosa SP, Dhainaut JF, Lopez-Rodriguez A, Steingrub JS, Garber GE, Helterbrand JD, Ely EW, Fisher CJ Jr (2001) Efficacy and safety of recombinant human activated protein C for severe sepsis. N Engl J Med 344:699–709
Kinasewitz GT, Yan SB, Basson B, Comp P, Russell JA, Cariou A, Um SL, Utterback B, Laterre PF, Dhainaut JF (2004) Universal changes in biomarkers of coagulation and inflammation occur in patients with severe sepsis, regardless of causative micro-organism [ISRCTN74215569]. Crit Care 8:R82–R90
Preston RJ, Villegas-Mendez A, Sun YH, Hermida J, Simioni P, Philippou H, Dahlback B, Lane DA (2005) Selective modulation of protein C affinity for EPCR and phospholipids by Gla domain mutation. FEBS J 272:97–108
Villegas-Mendez A, Montes R, Ambrose LR, Warrens AN, Laffan M, Lane DA (2007) Proteolysis of the endothelial cell protein C receptor by neutrophil proteinase 3. J Thromb Haemost 5:980–988
Acknowledgments
This work was supported by grants from l’Agence de Biomédecine, La Société de Néphrologie, l’Association pour le Développement de la Réanimation (ADR, Nantes), Lilly-France. This work was also in part supported by XENOME, an EU-funded Integrated Project in Life Sciences, Genomics and Biotechnology for Health (LSHB-CT-2006-037377) and by a grant from la Fondation de l’Avenir (contrat ET8-498).
Conflict of interest
The authors declare no competing financial interests.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Guitton, C., Gérard, N., Sébille, V. et al. Early rise in circulating endothelial protein C receptor correlates with poor outcome in severe sepsis. Intensive Care Med 37, 950–956 (2011). https://doi.org/10.1007/s00134-011-2171-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-011-2171-y