Abstract
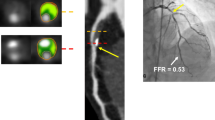
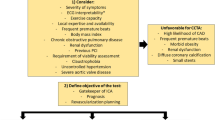
This review surveys the findings of the International Study of Comparative Health Effectiveness with Medical and Invasive Approaches (ISCHEMIA) trial and puts them into a clinical perspective regarding its effect of the role of cardiac magnetic resonance imaging (CMR) as a well-validated gatekeeper for invasive angiography and myocardial revascularization. Noninvasive stress testing of patients with intermediate-to-high pretest likelihood for obstructive coronary artery disease (CAD) using perfusion CMR provides excellent diagnostic accuracy in detecting ischemic myocardium, and additional information from tissue characterization can guide the management of patients with stable angina toward a more individualized therapy as other non-coronary underlying causes of chest pain can be detected. Since ISCHEMIA failed to show that an invasive strategy using percutaneous coronary intervention or coronary artery bypass grafting was associated with an improved prognosis compared with initial conservative medical therapy among stable patients with moderate-to-severe ischemia, CMR as a multifaceted diagnostic imaging approach to explain patients’ symptoms should be preferred over anatomical and stress testing alone. Nevertheless, the exclusion of left main coronary artery stenosis either by coronary CT or MR angiography may be required. In conclusion, the results of the ISCHEMIA trial are in good accordance with those of the MR-INFORM trial recently published in the New England Journal of Medicine, as the noninvasive management of a large proportion of patients with CAD was shown to be noninferior to current invasive strategies. Recent outcome data from trials may therefore have an impact on future guidelines to further reduce the execution of unnecessary left heart catheterizations.
Zusammenfassung
Im vorliegenden Übersichtsartikel werden die Ergebnisse der ISCHEMIA-Studie (International Study of Comparative Health Effectiveness with Medical and Invasive Approaches) genauer betrachtet und die daraus entstehenden Konsequenzen für die Kardio-Magnetresonanztomographie (MRT) als gut validiertem Gatekeeper für die invasive Angiographie und die myokardiale Revaskularisation aus klinischer Perspektive diskutiert. Der nichtinvasive Stresstest unter Verwendung der Perfusions-MRT bietet eine ausgezeichnete diagnostische Genauigkeit zum Nachweis von ischämischem Myokard bei Patienten mit mittlerer bis hoher Vortestwahrscheinlichkeit für eine stenosierende koronare Herzkrankheit (KHK). Zusätzliche Informationen aus der Gewebecharakterisierung können bei Patienten mit stabiler Angina pectoris zu einer individualisierteren Therapie führen, da weitere zugrunde liegende Ursachen für Brustschmerzen erkannt werden können. Da sich in der ISCHEMIA-Studie nicht nachweisen ließ, dass eine invasive Strategie mit perkutaner Koronarintervention oder Bypassoperation der Koronararterien mit einer verbesserten Prognose im Vergleich zur konservativen medizinischen Therapie bei stabilen Patienten mit mittelschwerer bis schwerer Ischämie verbunden war, sollte die Kardio-MRT als vielschichtiges diagnostisches Bildgebungsverfahren gegenüber den rein anatomischen und Belastungsuntersuchungen bevorzugt werden, um die Symptome von Patienten zu erklären. Möglicherweise muss zusätzlich der Ausschluss einer Stenose im linken Hauptstamm entweder durch Koronar-CT oder MR-Angiographie durchgeführt werden. Fazit ist, dass die Ergebnisse der ISCHEMIA-Studie gut mit denen der kürzlich im New England Journal of Medicine veröffentlichten MR-INFORM-Studie übereinstimmen, da das nichtinvasive Management den derzeitigen invasiven Strategien bei einem Großteil von Patienten mit KHK nicht unterlegen war. Die aktuellen Daten aus Outcome-Studien können daher Auswirkungen auf zukünftige Richtlinien haben, um die Durchführung unnötiger Linksherzkatheteruntersuchungen weiter zu reduzieren.



Similar content being viewed by others
Change history
01 July 2020
In the above mentioned article, the family name of the second author was not given correctly: it is Carerj instead of Careri.
The authors apologize for this mistake.
The original article has been …
References
Maron DJ, Hochman JS, Reynolds HR et al (2020) Initial invasive or conservative strategy for stable coronary disease. N Engl J Med 382:1395–1407. https://doi.org/10.1056/NEJMoa1915922
Spertus JA, Jones PG, Maron DJ et al (2020) Health-status outcomes with invasive or conservative care in coronary disease. N Engl J Med 382:1408–1419. https://doi.org/10.1056/NEJMoa1916370
Nagel E, Greenwood JP, McCann GP et al (2019) Magnetic resonance perfusion or fractional flow reserve in coronary disease. N Engl J Med 380:2418–2428. https://doi.org/10.1056/NEJMoa1716734
Nagel E, Klein C, Paetsch I et al (2003) Magnetic resonance perfusion measurements for the noninvasive detection of coronary artery disease. Circulation 108:432–437. https://doi.org/10.1161/01.CIR.0000080915.35024.A9
Lockie T, Ishida M, Perera D et al (2011) High-resolution magnetic resonance myocardial perfusion imaging at 3.0-Tesla to detect hemodynamically significant coronary stenoses as determined by fractional flow reserve. J Am Coll Cardiol 57:70–75. https://doi.org/10.1016/j.jacc.2010.09.019
Watkins S, McGeoch R, Lyne J et al (2009) Validation of magnetic resonance myocardial perfusion imaging with fractional flow reserve for the detection of significant coronary heart disease. Circulation 120:2207–2213. https://doi.org/10.1161/CIRCULATIONAHA.109.872358
Morton G, Chiribiri A, Ishida M et al (2012) Quantification of absolute myocardial perfusion in patients with coronary artery disease: comparison between cardiovascular magnetic resonance and positron emission tomography. J Am Coll Cardiol 60:1546–1555. https://doi.org/10.1016/j.jacc.2012.05.052
Schwitter J, Wacker CM, Wilke N et al (2013) MR-IMPACT II: Magnetic Resonance Imaging for Myocardial Perfusion Assessment in Coronary artery disease Trial: perfusion-cardiac magnetic resonance vs. single-photon emission computed tomography for the detection of coronary artery disease: a comparative multicentre, multivendor trial. Eur Heart J 34:775–781. https://doi.org/10.1093/eurheartj/ehs022
Greenwood JP, Herzog BA, Brown JM et al (2016) Cardiovascular magnetic resonance and single-photon emission computed tomography in suspected coronary heart disease. Ann Intern Med 165:830–831. https://doi.org/10.7326/L16-0480
Takx RAP, Blomberg BA, Aidi HE et al (2014) Diagnostic accuracy of stress myocardial perfusion imaging compared to invasive coronary angiography with fractional flow reserve meta-analysis. Circ Cardiovasc Imaging 8:e2666. https://doi.org/10.1161/CIRCIMAGING.114.002666
Kwong RY, Ge Y, Steel K et al (2019) Cardiac magnetic resonance stress perfusion imaging for evaluation of patients with chest pain. J Am Coll Cardiol 74:1741–1755. https://doi.org/10.1016/j.jacc.2019.07.074
Hachamovitch R, Hayes SW, Friedman JD et al (2003) Comparison of the short-term survival benefit associated with revascularization compared with medical therapy in patients with no prior coronary artery disease undergoing stress myocardial perfusion single photon emission computed tomography. Circulation 107:2900–2907. https://doi.org/10.1161/01.CIR.0000072790.23090.41
Shaw LJ, Berman DS, Picard MH et al (2014) Comparative definitions for moderate-severe ischemia in stress nuclear, echocardiography, and magnetic resonance imaging. JACC Cardiovasc Imaging 7:593–604. https://doi.org/10.1016/j.jcmg.2013.10.021
Knuuti J, Wijns W, Saraste A et al (2019) 2019 ESC guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J 41:407–477. https://doi.org/10.1093/eurheartj/ehz425
Neumann F‑J, Sousa-Uva M, Ahlsson A et al (2019) 2018 ESC/EACTS guidelines on myocardial revascularization. Eur Heart J 40:87–165. https://doi.org/10.1093/eurheartj/ehy394
Andresen D (2018) Deutscher Herzbericht 2018. Deutsche Herzstiftung, Frankfurt am Main
Nagel E (2010) Magnetic resonance coronary angiography: the condemned live longer. J Am Coll Cardiol 56:992–994. https://doi.org/10.1016/j.jacc.2010.02.069
Hendel RC, Friedrich MG, Schulz-Menger J et al (2016) CMR first-pass perfusion for suspected inducible myocardial ischemia. JACC Cardiovasc Imaging 9:1338–1348. https://doi.org/10.1016/j.jcmg.2016.09.010
Hinojar R, Varma N, Child N et al (2015) T1 mapping in discrimination of hypertrophic phenotypes: hypertensive heart disease and hypertrophic cardiomyopathy. Circ Cardiovasc Imaging 8:e3285. https://doi.org/10.1161/CIRCIMAGING.115.003285
Hinojar R, Foote L, Ucar E et al (2014) Myocardial T2 mapping for improved detection of inflammatory myocardial involvement in acute and chronic myocarditis. J Cardiovasc Magn Reson 16:O63. https://doi.org/10.1186/1532-429X-16-S1-O63
Puntmann VO, Carr-White G, Jabbour A et al (2018) Native T1 and ECV of noninfarcted myocardium and outcome in patients with coronary artery disease. J Am Coll Cardiol 71:766–778. https://doi.org/10.1016/j.jacc.2017.12.020
Puntmann VO, Carr-White G, Jabbour A et al (2016) T1-mapping and outcome in nonischemic cardiomyopathy. JACC Cardiovasc Imaging 9:40–50. https://doi.org/10.1016/j.jcmg.2015.12.001
Thygesen K, Alpert JS, Jaffe AS et al (2019) Fourth universal definition of myocardial infarction. Eur Heart J 40:237–269. https://doi.org/10.1093/eurheartj/ehy462
Pieske B, Tschöpe C, de Boer RA et al (2019) How to diagnose heart failure with preserved ejection fraction: the HFA-PEFF diagnostic algorithm: a consensus recommendation from the Heart Failure Association (HFA) of the European Society of Cardiology (ESC). Eur Heart J 40:3297–3317. https://doi.org/10.1093/eurheartj/ehz641
Zamorano JL, Lancellotti P, Rodriguez Muñoz D et al (2016) 2016 ESC position paper on cancer treatments and cardiovascular toxicity developed under the auspices of the ESC Committee for Practice Guidelines. Eur Heart J 37:2768–2801. https://doi.org/10.1093/eurheartj/ehw211
Douglas PS, Hoffmann U, Patel MR et al (2015) Outcomes of anatomical versus functional testing for coronary artery disease. N Engl J Med 372:1291–1300. https://doi.org/10.1056/NEJMoa1415516
SCOT-HEART Investigators, Newby DE, Adamson PD et al (2018) Coronary CT angiography and 5‑year risk of myocardial infarction. N Engl J Med 379:924–933. https://doi.org/10.1056/NEJMoa1805971
Kim WY, Danias PG, Stuber M et al (2001) Coronary magnetic resonance angiography for the detection of coronary stenoses. N Engl J Med 345:1863–1869. https://doi.org/10.1056/NEJMoa010866
Greenwood JP, Maredia N, Younger JF et al (2012) Cardiovascular magnetic resonance and single-photon emission computed tomography for diagnosis of coronary heart disease (CE-MARC): a prospective trial. Lancet 379:453–460. https://doi.org/10.1016/S0140-6736(11)61335-4
Zhang L, Song X, Dong L et al (2018) Additive value of 3T cardiovascular magnetic resonance coronary angiography for detecting coronary artery disease. J Cardiovasc Magn Reson 20:29. https://doi.org/10.1186/s12968-018-0450-2
Assomull RG, Shakespeare C, Kalra PR et al (2011) Role of cardiovascular magnetic resonance as a gatekeeper to invasive coronary angiography in patients presenting with heart failure of unknown etiology. Circulation 124:1351–1360. https://doi.org/10.1161/CIRCULATIONAHA.110.011346
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
E. Nagel received grant support from Bayer AG and speaker fees from Bayer AG. C.T. Arendt received a “Rotation Grant” from the DZHK. L. Careri and V.O. Puntmann declare that they have no competing interests.
For this article no studies with human participants or animals were performed by any of the authors. All studies performed were in accordance with the ethical standards indicated in each case.
Additional information
The original version of this article was revised: In this article, the family name of the second author was not given correctly: it is Carerj instead of Careri. The authors apologize for this mistake.
Rights and permissions
About this article
Cite this article
Nagel, E., Carerj, M.L., Arendt, C.T. et al. After ISCHEMIA: Is cardiac MRI a reliable gatekeeper for invasive angiography and myocardial revascularization?. Herz 45, 446–452 (2020). https://doi.org/10.1007/s00059-020-04936-w
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-020-04936-w