Abstract
Objectives
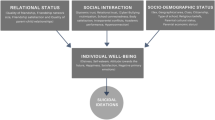
The aim of this study was to identify whether suicidal ideation in low-income adolescents is influenced by social environment and social support.
Methods
We performed a growth curve model using a sample of 6687 low-income adolescents living in the Mobile, AL Metropolitan Statistical Area. The outcome for the present study was whether the participant had thought about suicide in the past 12 months.
Results
From 1998 to 2011, an average of 14.3% of the study participants indicated that they had considered killing themselves in the past 12 months on an annual basis (11.2–17.6%). Accounting for confounding factors, positive peer support, inevitability of violence, and having moved in the past year resulted in an increased risk, though the effect of inevitability of violence decreased over time. Meanwhile, elevated perceptions of contextual safety and increased parental warmth resulted in reduced risk. These findings suggest that social support and social context are important indicators of suicidal ideation in adolescents.
Conclusions
Suicidal ideation is an important predictor of suicidal behavior. If suicidal ideation can be prevented, or predicted, then it is possible that suicidal behavior can be reduced.
Similar content being viewed by others
References
Aneshensel CS, Sucoff CA (1996) The neighborhood context of adolescent mental health. J Health Soc Behav 37:293–310. https://doi.org/10.2307/2137258
Baca-Garcia E, Perez-Rodriguez MM, Oquendo MA, Keyes KM, Hasin DS, Grant BF, Blanco C (2011) Estimating risk for suicide attempt: are we asking the right questions? Passive suicidal ideation as a marker for suicidal behavior. J Affect Disorders 134:327–332. https://doi.org/10.1016/j.jad.2011.06.026
Bandura A (1973) Aggression: a social learning analysis. Prentice Hall, Englewood Cliffs
Bolland JM, Lian BE, Formichella CM (2005) The origins of hopelessness among inner-city African-American adolescents. Am J Community Psychol 36:293–305. https://doi.org/10.1007/s10464-005-8627-x
Bolland JM, Bryant CM, Lian BE, McCallum DM, Vazsonyi AT, Barth JM (2007) Development and risk behavior among African American, Caucasian, and mixed-race adolescents living in high poverty inner-city neighborhoods. Am J Community Psychol 40:230–249. https://doi.org/10.1007/s10464-007-9132-1
Brausch AM, Decker KM, Hadley AG (2011) Risk of suicidal ideation in adolescents with both self-asphyxial risk-taking behavior and non-suicidal self-injury. Suicide Life-Threat 41:424–434. https://doi.org/10.1111/j.1943-278X.2011.00042.x
Browne DC, Clubb PA, Aubrecht AM, Jackson M (2001) Minority heath risk behaviors: an introduction to research on sexually transmitted diseases, violence, pregnancy prevention and substance use. Matern Child Health J 5:215–224. https://doi.org/10.1023/A:1013077404562
CDC (2013) Centers for Disease Control and Prevention. Web-based Injury Statistics Query and Reporting System (WISQARS) [Online]. National Center for Injury Prevention and Control, CDC. https://www.cdc.gov/injury/wisqars/index.html. Accessed 8 Aug 2018
Cukrowicz KC, Schlegel EF, Smith PN, Jacobs MP, Van Orden KA, Paukert AL, Pettit JW, Joiner TE (2011) Suicide ideation among college students evidencing subclinical depression. J Am Coll Health 59:1–33. https://doi.org/10.1080/07448481.2010.483710
Donath C, Graessel E, Baier D, Bleich S, Hillemacher T (2014) Is parenting style a predictor of suicide attempts in a representative sample of adolescents? BMC Pediatr 14:113. https://doi.org/10.1186/1471-2431-14-113
Farrell CT, Bolland JM, Cockerham WC (2015) The role of social support and social context on the incidence of attempted suicide among adolescents living in extremely impoverished communities. J Adolesc Health 56:59–65. https://doi.org/10.1016/j.jadohealth.2014.08.015
Fotti SA, Katz LY, Afifi TO, Cox BJ (2006) The associations between peer and parental relationships and suicidal behaviours in early adolescents. Can J Psychiat 51:698–703. https://doi.org/10.1177/070674370605101106
Glynn TJ (1981) Psychological sense of community: measurement and application. Hum Resour 34:789–818. https://doi.org/10.1177/001872678103400904
Harter S (1982) The perceived competence scale for children. Child Dev 53:87–97. https://doi.org/10.2307/1129640
Hooks B (1989) Talking back: thinking feminist, thinking black. South End Press, Boston
Joe S, Baser RS, Neighbors HW, Caldwell CH, Jackson JS (2009) 12-month and lifetime prevalence of suicide attempts among black adolescents in the National Survey of American Life. J Am Acad Child Adolesc Psychiatry 48:271–282. https://doi.org/10.1097/CHI.0b013e318195bccf
Kawachi I (2006) Social capital and health: making the connections one step at a time. Int J Epidemiol 35:989–993. https://doi.org/10.1093/ije/dyl117
Kazdin AE, Esveldt-Dawson K, Unis AS, Rancurello MD (1983) Child and parent evaluations of depression and aggression in psychiatric inpatient children. J Abnorm Child Psychol 11:401–413. https://doi.org/10.1007/BF00914248
Kerr DC, Preuss LJ, King CA (2006) Suicidal adolescents’ social support from family and peers: gender-specific associations with psychopathology. J Abnorm Child Psychol 34:99–110. https://doi.org/10.1007/s10802-005-9005-8
Kerr DC, Owen LD, Pears KC, Capaldi DM (2008) Prevalence of suicidal ideation among boys and men assessed annually from ages 9 to 29 years. Suicide Life-Threat 38:390–402. https://doi.org/10.1521/suli.2008.38.4.390
Kidd S, Henrich CC, Brookmeyer KA, Davidson L, King RA, Shahar G (2006) The social context of adolescent suicide attempts: interactive effects of parent, peer, and school social relations. Suicide Life-Threat 36:386–395. https://doi.org/10.1521/suli.2006.36.4.386
Klemera E, Brooks FM, Chester KL, Magnusson J, Spencer N (2017) Self-harm in adolescent: protective health assets in the family, school and community. Int J Public Health 62:631–638. https://doi.org/10.1007/s00038-016-0900-2
Lambert SF, Copeland-Linder N, Ialongo NS (2008) Longitudinal associations between community violence exposure and suicidality. J Adolesc Health 43:380–386. https://doi.org/10.1016/j.jadohealth.2008.02.015
Lamborn SD, Mounts NS, Steinberg L, Dornbusch SM (1991) Patterns of competence and adjustment among adolescents from authoritative, authoritarian, indulgent, and neglectful families. Child Dev 62:1049–1065. https://doi.org/10.1111/j.1467-8624.1991.tb01588.x
LaVome RW, Droege JR, Hipwell AE, Stepp SD, Keenan K (2016) Brief report: suicidal ideation in adolescent girls: Impact of race. J Adolesc 53:16–20. https://doi.org/10.1016/j.adolescence.2016.08.013
Lin N, Ensel WM, Simeone RS, Kuo W (1979) Social support, stressful life events, and illness: a model and an empirical test. J Health Soc Behav 20:108–119. https://doi.org/10.2307/2136433
Lowry R, Crosby AE, Brener ND, Kann L (2014) Suicidal thoughts and attempts among US high school students: trends and associated health-risk behaviors, 1991–2011. J Adolesc Health 54:100–108. https://doi.org/10.1016/j.jadohealth.2013.07.024
National Center of Health Statistics. Health, United States (2013) With special feature on prescription drugs. Hyattsville, MD 2014
Newman BM, Newman PR, Griffen S, O’Connor K, Spas J (2007) The relationship of social support to depressive symptoms during the transition to high school. Adolescence 42:441–459
O’Leary CC, Frank DA, Grant-Knight W, Beeghly M, Augustyn M, Rose-Jacobs R, Gannon K (2006) Suicidal ideation among urban nine and ten year olds. J Dev Behav Pediatr 27:33–39. https://doi.org/10.1097/00004703-200602000-00005
Prinstein MJ, Aikins JW (2004) Cognitive moderators of the longitudinal association between peer rejection and adolescent depressive symptoms. J Abnorm Child Psychol 32:147–158. https://doi.org/10.1023/B:JACP.0000019767.55592.63
QuickStats (2017) Suicide rates for teens aged 15–19 years, by sex—United States, 1975–2015. MMWR Morb Mortal Wkly Rep 66:816. https://doi.org/10.15585/mmwr.mm6630a6
Rigby K, Slee P (1999) Suicidal ideation among adolescent school children, involvement in bully—victim problems, and perceived social support. Suicide Life-Threat 29:119–130. https://doi.org/10.1111/j.1943-278X.1999.tb01050.x
SAMHSA (2014) Substance Abuse and Mental Health Services Administration. Results from the 2013 National Survey on Drug Use and Health: Mental Health Findings, NSDUH Series H-49. HHS Publication No. (SMA) 14-4887. https://www.samhsa.gov/data/sites/default/files/NSDUHmhfr2013/NSDUHmhfr2013.pdf. Accessed 8 Aug 2018
Schilling EA, Aseltine RH, Glanovsky JL, James A, Jacobs D (2009) Adolescent alcohol use, suicidal ideation, and suicide attempts. J Adolesc Health 44:335–341. https://doi.org/10.1016/j.jadohealth.2008.08.006
Spann M, Molock SD, Barksdale C, Matlin S, Puri R (2006) Suicide and African American teenagers: risk factors and coping mechanisms. Suicide Life-Threat 36:553–568
Spirito A, Brown L, Overholser J, Fritz G (1989) Attempted suicide in adolescence: a review and critique of the literature. Clin Psychol Rev 9:335–363. https://doi.org/10.1016/0272-7358(89)90061-5
Steinberg L (1990) Autonomy, conflict, and harmony in the family relationship. In: Feldman SS, Elliot GR (eds) At the threshold: the developing adolescent. Harvard University Press, Cambridge, pp 255–276
Turner HA, Finkelholder D, Shattuck A (2012) Recent victimization exposure and suicidal ideation in adolescents. Arch Pediatr Adolesc Med 166:1149–1154. https://doi.org/10.1001/archpediatrics.2012.1549
Yoon TH, Noh M, Han J, Jung-Choi K, Khang YH (2015) Deprivation and suicide mortality across 424 neighborhoods in Seoul, South Korea: a Bayesian spatial analysis. Int J Public Health 60:969–976. https://doi.org/10.1007/s00038-015-0694-7
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Institutional review board (IRB) approval was acquired from Western Kentucky University (Ref#: IRB 14-219). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the special issue “Adolescent transitions”.
Rights and permissions
About this article
Cite this article
Farrell, C.T., Moledina, Z. & Katta, M. Suicidal thoughts in low-income adolescents: a longitudinal analysis. Int J Public Health 64, 285–292 (2019). https://doi.org/10.1007/s00038-019-01201-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00038-019-01201-8