Abstract
Purpose
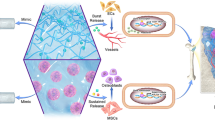
Previous attempts to stimulate angiogenesis have focused on the delivery of growth factors and cytokines, genes encoding for specific angiogenic inductive proteins or transcription factors, or participating cells. While high concentrations of bioactive glasses have exhibited osteogenic potential, recent studies have demonstrated that low concentrations of particular bioactive glasses are angiogenic. We hypothesized that a well known bioactive glass (Bioglass® 45S5) possesses proangiogenic potential over a limited range of concentrations.
Materials and Methods
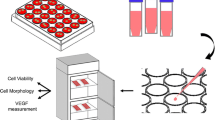
Varying amounts of Bioglass were loaded into absorbable collagen sponges. The proangiogenic potential of Bioglass was determined by examining the capacity of the soluble products to induce endothelial cell proliferation, tubule formation in a co-culture, and upregulate vascular endothelial growth factor (VEGF) production.
Results
We determined a range of Bioglass concentrations which exhibit proangiogenic potential. Furthermore, we demonstrated that the proangiogenic capacity of this material is related to the soluble dissolution products of Bioglass and the subsequent production of cell-secreted angiogenic factors by stimulated cells.
Conclusions
These studies suggest that this bioactive glass possesses a robust proangiogenic potential, and this strategy may provide an alternative to recombinant inductive growth factors.




Similar content being viewed by others
References
P. Carmeliet. Manipulating angiogenesis in medicine. J. Intern. Med. 255:538–561 (2004).
M. Nomi, A. Atala, P. D. Coppi, and S. Soker. Principals of neovascularization for tissue engineering. Mol. Aspects. Med. 23:463–483 (2002).
L. L. Hench, R. J. Splinter, W. C. Allen, and T. K. Greenlee. Bonding mechanisms at the interface of ceramic prosthetic materials. J. Biomed. Mater. Res. 5:117–141 (1971).
L. L. Hench, I. D. Xynos, and J. M. Polak. Bioactive glasses for in situ tissue regeneration. J. Biomater. Sci. Polym. Ed. 15:543–562 (2004).
E. J. Schepers, and P. Ducheyne. Bioactive glass particles of narrow size range for the treatment of oral bone defects: a 1–24 month experiment with several materials and particle sizes and size ranges. J. Oral. Rehabil. 24:171–181 (1997).
T. B. Lovelace, J. T. Mellonig, R. M. Meffert, A. A. Jones, P. V. Nummikoski, and D. L. Cochran. Clinical evaluation of bioactive glass in the treatment of periodontal osseous defects in humans. J. Periodontol. 69:1027–1035 (1998).
R. Mengel, D. Schreiber, and L. Flores-de-Jacoby. Bioabsorbable membrane and bioactive glass in the treatment of intrabony defects in patients with generalized aggressive periodontitis: results of a 5-year clinical and radiological study. J. Periodontol. 77:1781–1787 (2006).
M. Marcolongo, P. Ducheyne, J. Garino, and E. Schepers. Bioactive glass fiber/polymeric composites bond to bone tissue. J. Biomed. Mater. Res. 39:161–170 (1998).
J. A. Roether, A. R. Boccaccini, L. L. Hench, V. Maquet, S. Gautier, and R. Jerjme. Development and in vitro characterisation of novel bioresorbable and bioactive composite materials based on polylactide foams and Bioglass for tissue engineering applications. Biomaterials 23:3871–3878 (2002).
J. Yao, S. Radina, P. S. Leboy, and P. Ducheyne. The effect of bioactive glass content on synthesis and bioactivity of composite poly (lactic-co-glycolic acid)/bioactive glass substrate for tissue engineering. Biomaterials 26:1935–1943 (2005).
C. R. Perry. Bone repair techniques, bone graft, and bone graft substitutes. Clin. Orthop. Relat. Res. 360:71–86 (1999).
J. K. Leach, and D. J. Mooney. Bone engineering by controlled delivery of osteoinductive molecules and cells. Expert. Opin. Biol. Ther. 4:1015–1027 (2004).
I. D. Xynos, A. J. Edgar, L. D. Buttery, L. L. Hench, and J. M. Polak. Ionic products of bioactive glass dissolution increase proliferation of human osteoblasts and induce insulin-like growth factor II mRNA expression and protein synthesis. Biochem. Biophys. Res. Commun. 276:461–465 (2000).
I. D. Xynos, A. J. Edgar, L. D. Buttery, L. L. Hench, and J. M. Polak. Gene-expression profiling of human osteoblasts following treatment with the ionic products of Bioglass 45S5 dissolution. J. Biomed. Mater. Res. 55:151–157 (2001).
M. Bosetti, and M. Cannas. The effect of bioactive glasses on bone marrow stromal cells differentiation. Biomaterials 26:3873–3879 (2005).
S. Hattar, A. Asselin, D. Greenspan, M. Oboeuf, A. Berdal, and J. M. Sautier. Potential of biomimetic surfaces to promote in vitro osteoblast-like cell differentiation. Biomaterials 26:839–848 (2005).
E. Bergeron, M. E. Marquis, I. Chretien, and N. Faucheux. Differentiation of preosteoblasts using a delivery system with BMPs and bioactive glass microspheres. J. Mater. Sci. Mater. Med. 18:255–263 (2007).
H. Keshaw, A. Forbes, and R. M. Day. Release of angiogenic growth factors from cells encapsulated in alginate beads with bioactive glass. Biomaterials 26:4171–4179 (2005).
J. K. Leach, D. Kaigler, Z. Wang, P. H. Krebsbach, and D. J. Mooney. Coating of VEGF-releasing scaffolds with bioactive glass for angiogenesis and bone regeneration. Biomaterials 27:3249–3255 (2006).
R. M. Day. Bioactive glass stimulates the secretion of angiogenic growth factors and angiogenesis in vitro. Tissue Eng. 11:768–777 (2005).
W. H. Zhu, and R. F. Nicosia. The thin prep rat aortic ring assay: A modified method for the characterization of angiogenesis in whole mounts. Angiogenesis 5:81–86 (2002).
D. Donovan, N. J. Brown, E. T. Bishop, and C. E. Lewis. Comparison of three in vitro human ‘angiogenesis’ assays with capillaries formed in vivo. Angiogenesis 4:113–121 (2001).
S. Ivanovski, H. Li, T. Daley, and P. M. Bartold. An immunohistochemical study of matrix molecules associated with barrier membrane-mediated periodontal wound healing. J. Periodontal. Res. 35:115–126 (2000).
A. B. Ennett, D. Kaigler, and D. J. Mooney. Temporally regulated delivery of VEGF in vitro and in vivo. J. Biomed. Mater. Res. Part A 79A:176–184 (2006).
R. R. Chen, and D. J. Mooney. Polymeric growth factor delivery strategies for tissue engineering. Pharm. Res. 20:1103–1112 (2003).
S. R. Peyton, and A. J. Putnam. Extracellular matrix rigidity governs smooth muscle cell motility in a biphasic fashion. J. Cell Physiol. 204:198–209 (2005).
R. K. Willits, and S. L. Skornia. Effect of collagen gel stiffness on neurite extension. J. Biomater. Sci. Polym. Ed. 15:1521–1531 (2004).
N. Yamamura, R. Sudo, M. Ikeda, and K. Tanishita. Effects of the mechanical properties of collagen gel on the in vitro formation of microvessel networks by endothelial cells. Tissue Eng. 13:1443–1453 (2007).
T. Yeung, P. C. Georges, L. A. Flanagan, B. Marg, M. Ortiz, M. Funaki, N. Zahir, W. Ming, V. Weaver, and P. A. Janmey. Effects of substrate stiffness on cell morphology, cytoskeletal structure, and adhesion. Cell Motil. Cytoskeleton. 60:24–34 (2005).
S. X. Hsiong, P. Carampin, H. J. Kong, K. Y. Lee, and D. J. Mooney. Differentiation stage alters matrix control of stem cells. J. Biomed. Mater. Res. A (in press) (2007). DOI 10.1002/jbm.a.31521
A. J. Engler, S. Sen, H. L. Sweeney, and D. E. Discher. Matrix elasticity directs stem cell lineage specification. Cell 126:677–689 (2006).
C. B. Khatiwala, S. R. Peyton, M. Metzke, and A. J. Putnam. The regulation of osteogenesis by ECM rigidity in MC3T3-E1 cells requires MAPK activation. J. Cell Physiol. 211:661–672 (2007).
C. B. Khatiwala, S. R. Peyton, and A. J. Putnam. Intrinsic mechanical properties of the extracellular matrix affect the behavior of pre-osteoblastic MC3T3-E1 cells. Am. J. Physiol. Cell Physiol. 290:C1640–1650 (2006).
P. Carmeliet. Angiogenesis in health and disease. Nat. Med. 9:653–660 (2003).
T. P. Richardson, M. C. Peters, A. B. Ennett, and D. J. Mooney. Polymeric system for dual growth factor delivery. Nat. Biotechnol. 19:1029–1034 (2001).
C. R. Ozawa, A. Banfi, N. L. Glazer, G. Thurston, M. L. Springer, P. E. Kraft, D. M. McDonald, and H. M. Blau. Microenvironmental VEGF concentration, not total dose, determines a threshold between normal and aberrant angiogenesis. J. Clin. Invest. 113:516–527 (2004).
W. Helen, C. L. R. Merry, J. J. Blaker, and J. E. Gough. Three-dimensional culture of annulus fibrosus cells within PDLLA/Bioglass(R) composite foam scaffolds: Assessment of cell attachment, proliferation and extracellular matrix production. Biomaterials 28:2010–2020 (2007).
B. R. McAuslan, and W. Reilly. Endothelial cell phagokinesis in response to specific metal ions. Exp. Cell Res. 130:147–157 (1980).
K. S. Raju, G. Alessandri, M. Ziche, and P. M. Gullino. Ceruloplasmin, copper ions, and angiogenesis. J. Natl. Cancer Inst. 69:1183–1188 (1982).
C. K. Sen, S. Khanna, M. Venojarvi, P. Trikha, E. C. Ellison, T. K. Hunt, and S. Roy. Copper-induced vascular endothelial growth factor expression and wound healing. Am. J. Physiol. Heart Circ. Physiol. 282:H1821–1827 (2002).
M. Frangoulis, P. Georgiou, C. Chrisostomidis, D. Perrea, I. Dontas, N. Kavantzas, A. Kostakis, and O. Papadopoulos. Rat epigastric flap survival and VEGF expression after local copper application. Plast. Reconstr. Surg. 119:837–843 (2007).
Acknowledgements
The authors acknowledge financial support from the American Cancer Society and the Dean, UC Davis School of Medicine [notice ACS IRG-95-125-07] and David Fyhrie for use of mechanical testing equipment.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Leu, A., Leach, J.K. Proangiogenic Potential of a Collagen/Bioactive Glass Substrate. Pharm Res 25, 1222–1229 (2008). https://doi.org/10.1007/s11095-007-9508-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-007-9508-9