Summary
Objective
In the last decade, pharmacoeconomics has gained an increasing influence on the decisional process in the regulatory context of several European countries. The main aim of this analysis was to assess the quality of pharmacoeconomic evaluations enclosed by pharmaceutical companies in the pricing and reimbursement dossiers presented to the Italian Medicines Agency (AIFA).
Methods
A survey of pricing and reimbursement dossiers presented to AIFA between August 2004 (date of the agency’s institution) and November 2007 was conducted. According to Italian regulations concerning the submission of pharmacoeconomic information to national authorities, only those dossiers regarding the authorization of new chemical entities (never marketed before), orphan drugs for the treatment of rare diseases and those requiring the extension of therapeutic indications of already marketed drugs were selected for the survey. Data on both methodological features of pharmacoeconomic evaluations and overall features of clinical trials used as source of efficacy data for the economic analyses were collected. Some descriptive statistics of incremental cost-effectiveness ratios reported in the dossiers were also provided.
Results
In the time-span of about three years of AIFA activity, 109 dossiers have been reviewed and for 34 of them pharmaceutical companies provided also pharmacoecononomic analyses. Overall the production rate was 36% (39 out of 109 dossiers); as a matter of fact, a dossier may contain more than one pharmacoeconomic analysis (i.e. one for each therapeutic indication).
As expected, cost-effectiveness analysis is the most frequent type of economic evaluation (53.8%), followed by cost-utility analyses (20.5%). Cost-minimization analyses represent 25.6% of all economic evaluations, which is notably higher than the observed frequency in the international literature. Most economic evaluations were conducted for the assessment of new treatments for oncologic diseases or biotechnological products for rheumatic diseases, followed by drugs for infectious diseases (mostly AIDS) or neurological conditions.
The overall qualitative features of pharmacoeconomic evaluations in the dossiers appear to be highly variable, ranging from analyses meeting the highest methodological standards (especially in dossiers concerning medicines authorized via centralized procedure) to a dossier not providing basic information and describing the pharmacoeconomic results only in qualitative terms.
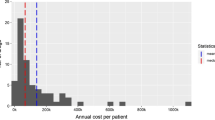
Based on drug prices submitted by pharmaceuticals manufacturers to AIFA, mean values of incremental cost-effectiveness ratios obtained after bootstrap resampling resulted € 17,907 per QALY (95% CI: 7,000–25,912) and € 41,676 per life-year saved (95% CI: 16,300–71,431).
Conclusions
Pharmacoeconomic techniques for health technology assessment of drug therapies need further development in the Italian context. In this perspective, the current survey of pharmacoeconomic evaluations enclosed in pricing and reimbursement dossiers could provide several suggestions.
Similar content being viewed by others
Bibliografia
Weinstein MC, Stason WB. Foundations of cost-effectiveness analysis for health and medical practices. N Engl J Med 1977; 296: 716–21
Torrance GW, Thomas WH, Sackett DL. A utility maximization model for evaluation of health care programs. Health Serv Res 1972; 7: 118–33
Oxman AD, Sackett DL, Guyatt GH. Users’ guides to the medical literature. I. How to get started. The Evidence-Based Medicine Working Group. JAMA 1993; 270: 2093–5
Jefferson T, Smith R, Yee Y, et al. Evaluating the BMJ guidelines for economic submission. JAMA 1996; 260: 275–7
Drummond MF, Jefferson TO. Guidelines for authors and peer reviewers of economic submissions to the BMJ. BMJ 1996; 313: 275–83
National Institute for Health and Clinical Excellence. Guide to the Methods of Technology Appraisal November 2007. UK: National Health Service, 2007
Pharmaceutical benefits pricing authority. Policies, procedures and methods used in the pricing of pharmaceutical products. Australia: PBPA, 2006
Spiegelhalter DJ, Abrams KR, Myles JP. Cost-Effectiveness, Policy-Making and Regulation. In: Bayesian Approaches to Clinical Trials and Health-care Evaluation. Chichester: John Wiley and Sons, 2004
Claxton K, Sculpher M, Drummond M. A rational framework for decision making by the national institute for clinical excellence (NICE). Lancet 2002; 360: 711–5
Neumann PJ, Rosen AB, Weinstein MC. Medicare and cost-effectiveness analysis. N Engl J Med 2005; 353: 1516–2211. Messori A, D’Alessandro P, Di Giorgio D, Tosolini F. Problems in Pharmacoeconomic Analyses (reply to editor). JAMA 2000: 284: 1923
Messori A, D’Alessandro P, Di Giorgio D, Tosolini F. Problems in Pharmacoeconomic Analyses (reply to editor). JAMA 2000: 284: 1923
Tengs TO, Adams ME, Pliskin JS, et al. Five-hundred life-saving interventions and their cost-effectiveness. Risk Anal 1995; 15: 369–90
Chaudhary MA, Stearns SC. Estimating confidence intervals for cost-effectiveness ratios: an example from a randomized trial. Stat Med 1996; 15: 1447–58
Briggs AH, Gray AM. Handling uncertainty when performing economic evaluation of healthcare interventions. Health Technol Assess 1999; 3: 1–134
Malone DC. Using indirect comparisons in pharmacoeconomic studies: time for implementation. Clin Ther 2007; 29: 2454–5
Ades AE, Sculpher M, Sutton A, et al. Bayesian methods for evidence synthesis in cost-effectiveness analysis. Pharmacoeconomics 2006; 24: 1–19
Hill SR, Mitchell AS, Henry DA. Problems with the interpretation of pharmacoeconomic analyses: a review of submissions to the Australian Pharmaceutical Benefits Scheme. JAMA 2000; 283: 2116–21
Pharmaceutical Benefits Advisory Committee. Guidelines for preparing submissions to the Pharmaceutical Benefits Advisory Committee (Version 4.1) December 2006. Australian Government, Department of Health and Ageing: Commonwealth of Australia, 2006
Hoffmann C, Graf von der Schulenburg JM on behalf of the Euromet group. The influence of economic evaluation studies on decision making. A European survey. Health Policy 2000; 52: 179–92
Freemantle N, Mason J. Publication bias in clinical trials and economic analyses. Pharmacoeconomics 1997; 12: 10–6
EFPIA (The European Federation of Pharmaceutical Industries and Associations). The Pharmaceutical Industry in Figures. EFPIA: 2007 update
Sculpher MJ, Pang FS, Manca A, et al. Generalisability in economic evaluation studies in healthcare: a review and case studies. Health Technol Assess 2004; 8: iii–iv, 1–192
Cornago D, Li Bassi L, De Compadri P, Garattini L. Pharmacoeconomic studies in Italy: a critical review of the literature. Eur J Health Econ 2007; 8: 89–95
Detsky AS, Laupacis A. Relevance of cost-effectiveness analysis to clinicians and policy makers. JAMA 2007; 298: 221–4
Stahl JE. Modelling methods for pharmacoeconomics and health technology assessment. Pharmacoeconomics 2008; 26: 131–48
Rennie D, Luft HS. Pharmacoeconomic analyses, making them transparent, making them credible. JAMA 2000; 283: 2158–60
Lucioni C, Ravasio R. Come valutare i risultati di uno studio farmacoeconomico? Pharmacoeconomics-Italian Research Articles 2004; 6:121–30
European value of a quality adjusted life year [online] (URL: http://research.ncl.ac.uk/eurovaq; accesso verificato al febbraio 2008)
Brouwer W, van Exel J, Baker R, Donaldson C. The new myth, the social value of the QALY. Pharmacoeconomics 2008; 26: 1–4
Claxton K, Briggs A, Buxton MJ, et al. Value based pricing for NHS drugs: an opportunity not to be missed? BMJ 2008; 336: 251–4
Donaldson C, Currie G, Mitton C. Cost effectiveness analysis in health care: contraindications. BMJ 2002; 325: 891–4
Friedberg M, Saffran B, Stinson TJ, et al. Evaluation of conflict of interest in economic analyses of new drugs used in oncology. JAMA 1999; 282: 1453–7
Hillman AL, Eisenberg JM, Pauly MV, et al. Avoiding bias in the conduct and reporting of cost-effectiveness research sponsored by pharmaceutical companies. N Engl J Med 1991; 324: 1362–5
Sassi F. Politiche editoriali per la valutazione economica: un passo avanti, due passi indietro? Non solo conflitto di interesse. Mecosan 1995; 4: 50–3
Attanasio E. Politiche editoriali per la valutazione economica: un passo avanti, due indietro? Gli interessi fanno parte del gioco. Mecosan 1995; 4: 59–60
Agenzia Italiana del Farmaco. Independent research on drugs funded by the Italian Medicines Agency (URL: http://www.agenziafarmaco.it/ accesso verificato al febbraio 2008)
Pearson SD, Rawlins MD. Quality, innovation, and value for money. NICE and the British National Health Service. JAMA 2005; 294: 2618–22
Taylor RS, Drummond MF, Salkeld G, Sullivan SD. Inclusion of cost effectiveness in licensing requirements of new drugs: the fourth hurdle. BMJ 2004; 329: 972–5
Agenzia Italiana del Farmaco. Criteri per l’attribuzione del grado di innovazione terapeutica dei nuovi farmaci. (URL: http://www.agenziafarmaco.it/allegati/documento_integrale.pdf accesso verificato al febbraio 2008)
Garattini L, Cornago D, De Compadri P. Pricing and reimbursement of in-patent drugs in seven European countries: a comparative analysis. Health Policy 2007; 82: 330–9
Collier J. The pharmaceutical price regulation scheme. Proposals for a new drug pricing mechanism in the NHS are welcomed. BMJ 2007; 334: 435–6
Author information
Authors and Affiliations
Corresponding author
Additional information
I contenuti del presente articolo riflettono la libera espressione e opinione dell’autore e non esprimono in alcun caso la posizione ufficiale dell’Agenzia Italiana del Farmaco.
Rights and permissions
About this article
Cite this article
Russo, P. La valutazione farmacoeconomica nel contesto regolatorio italiano. Pharmacoeconomics-Ital-Res-Articles 10, 59–75 (2008). https://doi.org/10.1007/BF03320643
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03320643