Abstract
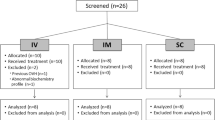
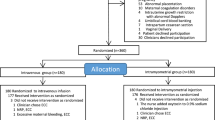
This prospective, randomised, double-blind study compared PCA fentanyl with PCA morphine for post-Caesarean section analgesia. Following a standardised general anaesthetic, 37 women were allocated to receive either fentanyl (n = 18) or morphine (n = 19). The PCA was commenced after the women had been made comfortable in the postanaesthetic recovery room with the appropriate opioid solution (mean dose required = fentanyl 375 μg or morphine 16 mg). Initial PCA settings were bolus 1 ml (fentanyl 25 μg or morphine 1 mg), lockout time ten minutes, and no background infusion. Both analgesic solutions provided effective analgesia for a mean of 37 hr with high levels of patient satisfaction, and there were no differences in VAS scores for pain and patient satisfaction, or for side effects (nausea, itch, and sleepiness) between fentanyl or morphine. However, more patients in the fentanyl group required supplementary boluses or alterations to the PCA settings (13/18 vs 4/19: P = 0.005), and one patient was removed from the study due to inadequate analgesia. We conclude that fentanyl is not recommended for routine PCA use following Caesarean section.
Résumé
Cette étude randomisée et à double aveugle compare la PCA au fentanyl avec la PCA à la morphine pour l’analgésie postcésarienne. Après une anesthésie générate standard, 37 femmes sont réparties pour recevoir soil du fentanyl (n = 18) soil de la morphine (n = 19). La PCA est debutée à la salle de réveil des que les patientes se sentent confortables sous une solution appropriée de morphinique (dose moyenne requise, fentanyl 375 μg ou morphine 16 mg). Le régime initial consiste en un bolus d’un ml (fentanyl 25 μg ou morphine 1 mg), un intervalle de sécurité de dix minutes, sans perfusion continue. Les deux solutions produisent une analgésie satisfaisante pour 37 h en moyenne avec un degré élevé de satisfaction pour la patiente, et on ne note pas de différence entre le fentanyl et la morphine pour l’évaluation de la douleur par EVA, le degré de satisfaction, et pour les effets secondaires (nausée, prurit et somnolence). Cependant, plus de patientes sous fentanyl ont eu besoin de bolus supplémentaires ou des modifications aux réglages de la PCA (13/18 vs 4/19; P = 0,005). Une patiente est exclue de l’étude pour raison d’insuffisance d’analgésie. En conclusion, nous ne recommandons pas la PCA au fentanyl après la césarienne.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Eisenach JC, Grice SC, Dewan DM. Patient-controlled analgesia following cesarean section: a comparison with epidural and intramuscular narcotics. Anesthesiology 1988; 68: 444–8.
Harrison DM, Sinatra R, Morgese L, Chung JH. Epidural narcotic and patient-controlled analgesia for postcesarean section pain relief. Anesthesiology 1988; 68: 454–7.
McCoy EP, Furness G, Wright PMC. Patient-controlled analgesia with and without background infusion. Analgesia assessed using the demand:delivery ratio. Anaesthesia 1993; 48: 256–60.
Owen H, Szekely SM, Plummer JL, Cushnie JM, Mather LE. Variables of patient-controlled analgesia 2. Concurrent infusion. Anaesthesia 1989; 44: 11–3.
Ready LB. Patient-controlled analgesia — does it provide more than comfort? (Editorial). Can J Anaesth 1990; 37: 719–21.
Rowbotham DJ. The development and safe use of patientcontrolled analgesia (Editorial). Br J Anaesth 1992; 331–2.
Sharma SK, Davies MW. Patient-controlled analgesia with a mixture of morphine and droperidol. Br J Anaesth 1993; 71: 435–6.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Howell, P.R., Gambling, D.R., Pavy, T. et al. Patient-controlled analgesia following caesarean section under general anaesthesia: a comparison of fentanyl with morphine. Can J Anaesth 42, 41–45 (1995). https://doi.org/10.1007/BF03010570
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03010570