Abstract
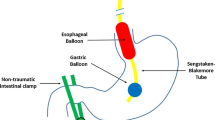
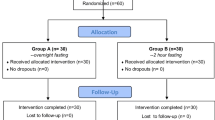
The efficacy of aspiration of gastric contents to reduce post-operative nausea and vomiting was investigated in a controlled randomized, double-blind study of 265 outpatients. Patients in the treated group had their stomachs aspirated with an orogastric tube. In the control group no tube was inserted. Data on the incidence of nausea and vomiting were collected in the recovery room, the day surgery unit and the day after surgery. The overall incidence of postoperative nausea and vomiting was comparable in the two groups. It was also comparable in the recovery room and the day surgery unit. However, treated patients had a higher incidence of both nausea (26.5% vs 12.0%,P < 0.005) and vomiting (16.7% vs 6.8%, P < 0.02) after their discharge from the day surgery unit. We conclude that aspiration of gastric contents with an orogastric tube does not decrease postoperative nausea and vomiting in outpatients and may increase it after discharge of the patient.
Résumé
L’efficacité de l’aspiration du contenu gastrique dans le but de réduire l’incidence des nausées et des vomissements post-opératoires a été évaluée au cours d’une étude contrôlée ran-domisée à double insu chez 265 patients dans un centre de chirurgie d’un jour. L’estomac des patients du groupe traité a été aspiré avec une sonde gastrique alors que dans le groupe témoin on n’a pas inséré de sonde. Les données concernant l’incidence des nausées et des vomissements ont été recueillies à la salle de réveil, à l’unité de chirurgie d’un jour et le len-demain de la chirurgie. L’incidence totale des nausées et vomissements fut comparable dans les deux groupes. Il n’y a pas eu non plus de différence à la salle de réveil et à l’unité de chirurgie d’un jour. Cependant, les patients traités ont présenté une incidence plus élevée de nausées (26,5% vs 12,0%,P <0,005) et vomissements (16,7% vs 6,8%, P < 0,02) après leur départ de l’unité de chirurgie d’un jour. Nous concluons que l’aspiration du contenu gastrique ne diminue pas l’incidence des nausées et vomissements postopératoires chez les patients de chirurgie d’un jour. En réalité, cette manoeuvre semble augmenter l’incidence de cette complication après le départ de l’unité chirurgicale.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Palazzo MGA, Strunin L. Anaesthesia and emesis. I. Etiology. Can Anaesth Soc J 1984; 31: 178–87.
Palazzo MGA, Strunin L. Anaesthesia and emesis. II. Prevention and management. Can Anaesth Soc J 1984; 31:407–15.
Meridy HW. Criteria for selection of ambulatory surgical patients and guidelines for anesthetic management: a retrospective study of 1553 cases. Anesth Analg 1982; 61: 921–6.
Gold BS, Kitz DS, Lecky JH, Neuhaus JM. Unanticipated admission to the hospital following ambulatory surgery. JAMA 1989; 262: 3008–10.
White PF, Shafer A. Nausea and vomiting: causes and prophylaxis. Seminars in Anesthesia 1987; 6: 300–8.
Burtles R, Peckett BW. Postoperative vomiting. Some factors affecting its incidence. Br J Anaesth 1957; 29: 114–23.
Smessaert A, Schehr CA, Artusio JF Jr. Nausea and vomiting in the immediate postanesthetic period. JAMA 1959; 170: 2072–6.
Dent SJ, Ramachandra V, Stephen CR. Postoperative vomiting: incidence, analysis, and therapeutic measures in 3000 patients. Anesthesiology 1955; 16: 564–72.
Holmes CM. Post-operative vomiting after ether/air anaesthesia. Anaesthesia 1965; 20: 199–206.
Cotter J. Complications of recovery from anesthesia.In: Hazards and Complications of Anaesthesia. London: Churchill Livingstone, 1987: 294–310.
Hovorka J, Korttila K, Erkola O. Gastric aspiration at the end of anaesthesia does not decrease postoperative nausea and vomiting. Anaesth Intensive Care 1990; 18: 58–61.
Knapp MR, Beecher HK. Postanaesthetic nausea, vomiting, and retching. Evaluation of the antiemitic drugs dimenhydrinate (dramamine), chlorpromazine, and pentobarbital sodium. JAMA 1956; 160: 376–85.
Bellville JW, Bross IDJ, Howland WS. Postoperative nausea and vomiting. IV: Factors related to postoperative nausea and vomiting. Anesthesiology 1960; 21: 186–93.
Riding JE. The prevention of postoperative vomiting. Br J Anaesth 1963; 35: 180–8.
Nelson PS, Streisand JB, Mulder SM, Pace NL, Stanley TH. Comparison of oral transmucosal fentanyl citrate and an oral solution of meperidine, diazepam, and atropine for premedication in children. Anesthesiology 1989; 70: 616–21.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Trépanier, C.A., Isabel, L. Perioperative gastric aspiration increases postoperative nausea and vomiting in outpatients. Can J Anaesth 40, 325–328 (1993). https://doi.org/10.1007/BF03009630
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03009630