Abstract
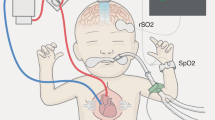
To examine the effects of low-flow cardiopulmonary bypass (CPB) and circulatory arrest (PHCA) on cerebral pressure-flow velocity relationships, we studied 32 patients (<9 mo of age) undergoing corrective cardiac procedures. Pressure-flow velocity relationships were studied during profound hypothermia (nasopharyngeal temperature <20° C). Cerebral blood-flow velocity (CBFV) was measured in the middle cerebral artery using transcranial Doppler sonography. The anterior fontanel pressure (AFP) was measured using an intracranial pressure monitor. Cerebral perfusion pressure (CPP) was calculated (mm Hg) as mean arterial pressure (MAP) minus AFP. Nasopharyngeal temperature, PaCO2 and haematocrit were controlled during the study period. Alpha-stat acid-base management was employed. The CBFV measurements were made continuously over a range of CPP as pump flow (Q) was decreased to low-flow or to circulatory arrest and again during the subsequent increase in Q and CPP to normal. As Q and CPP were increased after a period of low-flow CPB during which period detectable CBFV was present, the CBFV was greater at any given CPP than prior to the low-flow state (P < 0.05). However, after PHCA a higher CPP (P < 0.05) was necessary to re-establish detectable CBFV and at any given CPP the CBFV was less than prior to PHCA (P < 0.05). Seventeen patients underwent low-flow CPB during which CBFV became non-detectable (7 ± 1 cm · sec−1). In 12 of these patients the pattern of recovery of CBFV was the same as that observed after low-flow CPB whereas the remaining five (29%) demonstrated a pattern of recovery identical to the ones recorded after PHCA, We conclude that after PHCA a higher CPP is necessary to re-establish and maintain detectable CBFV. Furthermore, during low-flow CPB, patients where CBFV becomes non-detectable and show a pattern of CBFV recovery similar to PHCA, cessation of cerebral perfusion must be considered.
Résumé
Pour évaluer les effets de la circulation extracorporelle (CEC) à bas débit et de l’arrêt circulatoire sur la relation entre la vélocité et le débit sanguin, nous avons étudié 32 patients de moins de neuf mois soumis à des interventions cardiaques pour correction de malformations congénitales. Cette étude été réalisée sous l’hypothermie profonde (température nasale <20° C). La vélocité du débit sanguin cérébral (VDSC) a été mesurée dans l’artère cérébrale moyenne au moyen de l’ultrasonographie Döppler. La pression de la fontanelle antérieure (PFA) a été évaluée à l’aide d’un moniteur de pression intracrânienne. La pression de perfusion cérébrale (PPC) a été calculée en mm Hg en soustrayant la PFA de la pression artérielle moyenne (PAM), La température nasopharyngée, la PaCO2 et l’hématocrite ont été contrôlés pendant la période d’étude. Le système alpha-stat a été utilisé pour tes gaz artériels (mesurés à 37° C, non corrigés pour la température corporelle). Les mesures de VDSC ont été réalisées continuellement sur une gamme étendue de PPC alors que le débit de pompe (Q) était diminué jusqu’à l’arrêt circulatoire. Ces mesures ont été répétées pendant l’augmentation subséquente de Q et de la PPC jusqu’au retour à la normale. Alors que Q et la PPC étaient augmentés après une période de CBC à bas débit au cours de laquelle la VDSC était encore détectable, celle-ci a été plus élevée pour une PPC donnée qu’avant la période de bas débit (P < 0,05). Cependant, après arrð circulatoire, une PPC plus élevée (P < 0,05) a été nécessaire pour rétablir une VDSC détectable; pour une PPC donnée, le VDSC a toujours été plus basse qu’avant l’arrêt circulatoire (P < 0,05). Dix-sept patients ont été perfusés sous CEC à bas débit pendant laquelle on n’a pu détecter de VDSC (seuil de détectabilité > 7 ± 1 cm · sec−1). Chez 12 de ces patients, le pattern de la récupération de la VDSC était le même que celui qui est observé après des CEC à bas débits, alors que les cinq autres (29%) montraient un pattern de récupération identique que celui qu’on retrouvait après un arrêt circulatoire. Nous concluons qu’après arrêt circulatoire, une PPC plus élevée est nécessaire pour rétablir et maintenir une VDSC détectable. De plus, durant la CEC à bas débit, les malades où la VDSC devient indétectable et qui montrent un pattern de récupération semblable à l’arrêt circulatoire, un arrêt de la perfusion cérébrale doit être mis en cause.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Fox LS, Blackstone RH, Kirklin JW, Bishop SP, Bergdahl LA, Bradley EL. Relationship of brain blood flow and oxygen consumption to perfusion flow rate during profoundly hypo-thermic cardiopulmonary bypass. An experimental study. J Thorac Cardiovasc Surg 1984; 87: 658–64.
Rebeyka IM, Coles JG, Wilson GJ, el al. The effect of low-flow cardiopulmonary bypass on cerebral function: an experimental and clinical study. Ann Thorac Surg 1987; 43: 391–6.
Greeley WJ, Ungerleider RM, Kern FH, Brusino FG, Smith LR, Reves JG. Effects of cardiopulmonary bypass on cerebral blood flow in neonates, infants, and children. Circulation 1989; 80 (Suppl I): 1209–15.
Hillier SC, Burrows FA, Bissonnette B, Taylor RH. Cerebral hemodynamics in neonates and infants undergoing cardiopulmonary bypass and profound hypothermic circulatory arrest: assessment by transcranial Doppler sonography. Anesth Analg 1991; 72: 723–8.
Remington JW. Hysteresis loop behavior of the aorta and other extensible tissues. Am J Physiol 1955; 180: 83–95.
Remington JW, Alexander RS. Relation of tissue extensibility to smooth muscle tone. Am J Physiol 1956; 185: 302–8.
Remington JW. Extensibility behavior and hysteresis phenomena in smooth muscle tissues.In: Remington JW (Ed.). Tissue Elasticity. Washington, D.C.: American Physiological Society, 1957: 138–53.
van der Linden J, Wesslén Ö, Ekroth R, Tydén H, von Ahn H. Transcranial Doppler-estimated versus thermodilution-estimated cerebral blood flow during cardiac operations: influence of temperature and arterial carbon dioxide tension. J Thorac Cardiovasc Surg 1991; 102: 95–102.
van der Linden J, Priddy R, Ekroth R, et al. Cerebral perfusion and metabolism during profound hypothermia in children: a study of middle cerebral artery ultrasonic variables and cerebral extraction of oxygen. J Thorac Cardiovasc Surg 1991; 102: 103–14.
Taylor RH, Burrows FA, Bissonnette B. No flow during low-flow cardiopulmonary bypass (letter). J Thorac Cardiovasc Surg 1991; 101:362–4.
Taylor RH, Burrows FA, Bissonnette B. Cerebral pressure-flow velocity relationship during hypothermic cardiopulmonary bypass in neonates and infants. Anesth Analg 1992; 74: 636–42.
Stow PJ, Burrows FA, McLeod ME, Coles JG. The effect of cardiopulmonary bypass and profound hypothermic circulatory arrest on anterior fontanel pressure in infants. Can J Anaesth 1987; 34: 450–4.
Keenan NK, Taylor MJ, Coles JG, Prieur BJ, Burrows FA. The use of visual evoked potentials in assessing cardiopulmonary bypass and circulatory arrest. Electroencephalogr Clin Neurophysiol 1987; 68: 214–6.
Burrows FA, Hillier SC, McLeod ME, Irons KS, Taylor MJ. Anterior fontanel pressure and visual evoked potentials in neonates and infants undergoing profound hypothermic circulatory arrest. Anesthesiology 1990; 73: 632–6.
Carpenter MB, Sutin J. Human Neuroanatomy (8th ed.). Baltimore: Williams & Wilkins, 1983: 872.
Greeley WJ, Kern FH, Ungerleider RM, et al. The effect of hypothermic cardiopulmonary bypass and total circulatory arrest on cerebral metabolism in neonates, infants, and children. J Thorac Cardiovasc Surg 1991; 101: 783–94.
Reimer H, Burrows FA, Bissonnette B. Cerebral metabolism during low-flow cardiopulmonary bypass and profound hypothermic circulatory arrest. Anesthesiology 1992; 77: A1135.
Lupton BA, Hill A, Roland EH, Whitfield MF, Flodmark O. Brain swelling in the asphyxiated term newborn. Pathogenesis and outcome. Pediatrics 1988; 82: 139–46.
Ferry PC. Neurological sequelae of open-heart surgery in children. An “irritating question.” Am J Dis Child 1990; 144: 369–73.
Wantanabe T, Orita H, Kobayashi M, Washio M. Brain tissue pH, oxygen tension, and carbon dioxide tension in profoundly hypothermic cardiopulmonary bypass. Comparative study of circulatory arrest, nonpulsatile low-flow perfusion, and pulsatile low-flow perfusion. J Thorac Cardiovasc Surg 1989; 97: 396–401.
Rossi R, Ekroth R, Thompson RJ. No flow or low flow? A study of the ischaemic marker creatine kinase BB after deep hypothermic procedures. J Thorac Cardiovasc Surg 1989; 98: 193–9.
Lundar T, Lindberg H, Lindegaard K-F, et al. Cerebral perfusion during major cardiac surgery in children. Pediatr Cardiol 1987; 8: 161–5.
Preisen RH, Thieme R. Changes in fontanel pressure during cardiopulmonary bypass and profound hypothermic circulatory arrest in infants. Anesth Analg 1987; 66: 94–6.
Vidyasagar D, Raju TNK. A simple non-invasive technique of measuring intracranial pressure in the newborn. Pediatrics 1977; 59: 957–61.
Hill A, Volpe JJ. Measurement of intracranial pressure using the Ladd intracranial pressure monitor. J Pediatr 1981; 98: 974–6.
Jonas RA, Hickey P. Invited letter concerning: No flow during cardiopulmonary bypass. J Thorac Cardiovasc Surg 1991; 101: 364–5.
Leon JE, Bissonnette B. Cerebral vascular responses to carbon dioxide in children anaesthetized with halothane and isoflurane. Can J Anaesth 1991; 38: 817–26.
Pilato MA, Bissonnette B, Lerman J. Transcranial Doppler: response of cerebral blood flow velocity to carbon dioxide in anaesthetized children. Can J Anaesth 1991; 38: 37–42.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Burrows, F.A., Bissonnette, B. Cerebral blood flow velocity patterns during cardiac surgery utilizing profound hypothermia with lowflow cardiopulmonary bypass or circulatory arrest in neonates and infants. Can J Anaesth 40, 298–307 (1993). https://doi.org/10.1007/BF03009626
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03009626