Summary
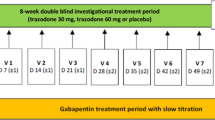
The effect of the non-tricyclic antidepressant mianserin on symptoms of diabetic neuropathy has been studied in 18 patients in a double-blind, cross-over study with imipramine as a positive control. The patients were treated with placebo, mianserin, and imipramine, each for two weeks, in randomized order, with 1–3 weeks between the treatments. The symptoms were assessed by observer and self-rating scales. Mianserin was given in the fixed dosage of 60 mg per day, whereas the dose of imipramine was adjusted to yield the optimal plasma concentration of imipramine plus desipramine of 400–600 nmol · l−1. The mianserin plus desmethylmianserin plasma concentration ranged from 85 to 850 nmol · l−', with the highest concentration in a patient who was a poor metabolizer of both sparteine and mephenytoin.
The symptoms of neuropathy were significantly reduced during imipramine treatment, although somewhat less than in earlier studies. In contrast, mianserin produced no change in symptoms in comparison with placebo. As there was no evidence that higher mianserin (plus metabolite) steady-state concentrations were associated with a more favourable effect, the negative outcome appeared not to be related to underdosing with mianserin. In contrast to drugs with documented effects on the symptoms of diabetic neuropathy, mianserin has a very weak or no inhibitory effect on 5-HT and noradrenaline reuptake and this may explain its poor clinical effect.
Similar content being viewed by others
References
Kvinesdal B, Molin J, Frøland A, Gram LF (1984) Imipramine treatment of painful diabetic neuropathy. J Am Med Assoc 251: 1727–1730
Gomez-Perez FJ, Rull JA, Dies H, Rodriguez-Rivera G, Gonzalez-Barranco J, Lozano-Castaneda O (1985) Nortriptyline and fluphenazine in the symptomatic treatment of diabetic neuropathy. A double-blind cross-over study. Pain 23: 395–400
Max MB, Culnane M, Schafer SC, Gracely RH, Walther DJ, Smoller B, Dubner R (1987) Amitriptyline relieves diabetic neuropathy pain in patients with normal or depressed mood. Neurology 37: 589–596
Sindrup SH, Gram LF, Skjold T, Grodum E, Brøsen K, Beck-Nielsen H (1990) Clomipramine vs desipramine vs placebo in the treatment of diabetic neuropathy symptoms. A double-blind cross-over study. Br J Clin Pharmacol 30: 683–691
Gram LF (1983) Antidepressants: receptors, pharmacokinetics and clinical effects. In: Burrows GD, Norman T, Davies B (eds) Antidepressants, Elsevier, Amsterdam, pp 81–95
Biegon A, Samuel D (1979) The in vivo distribution of an antidepressant drug (DMI) in male and female rats. Psychopharmacology 65: 259–263
Biegon A, Samuel D (1980) Interaction of tricyclic antidepressants with opiate receptors. Biochem Pharmacol 29: 460–462
Hall H, Ögren SO (1981) Effects of antidepressant drugs on different receptors in the brain. Eur J Pharmacol 70: 393–407
Sindrup SH, Gram LF, Brøsen K, Eshøj O, Mogensen EF (1990) The selective serotonin reuptake inhibitor paroxetine is effective in the treatment of diabetic neuropathy symptoms. Pain 42:135–144
Young RJ, Clarke BF (1985) Pain relief in diabetic neuropathy: the effectiveness of imipramine and related drugs. Diabetic Medicine 2: 363–366
Baumann P, Maitre L (1977) Blockade of presynaptic α-receptors and amine uptake in the rat brain by the antidepressant mianserin. NS Arch Pharmacol 300: 31–37
Sindrup SH, Brøsen K, Gram LF (1990) Nonlinear kinetics of imipramine in low and medium plasma level ranges. Ther Drug Monit 12: 445–449
Sindrup SH, Gram LF, Skjold T, Frøland A, Beck-Nielsen H (1990) Concentration-response relationship in imipramine treatment of diabetic neuropathy symptoms. Clin Pharmacol Ther 47: 509–516
Brøsen K, Otton SV, Gram LF (1985) Sparteine oxidation polymorphism in Denmark. Acta Pharmacol Toxicol 57: 357–360
Wedlund PJ, Aslanian WS, McAllister CB, Wilkinson GR, Branch RA (1984) Mephenytoin hydroxylation deficiency in Caucacians: frequency of a new oxidative drug metabolism polymorphism. Clin Pharmacol Ther 36: 773–780
Brøsen K, Otton SV, Gram LF (1986) Imipramine demethylation and hydroxylation: impact of the sparteine phenotype. Clin Pharmacol Ther 40: 543–549
Gram LF, Bjerre M, Kragh-Sorensen P, Kvinesdal B, Molin J, Pedersen OL, Reisby N (1983) Imipramine metabolites in the blood of patients during therapy and after overdose. Clin Pharmacol Ther 33: 335–342
Fields HL, Basbaum AI (1984) Endogenous pain control mechanisms. In: Wall PD, Melzach R (eds) Textbook of pain. Churchill Livingstone, London, pp 142–152
Lynch S, Max MB, Muir J, Smoller B, Dubner R (1990) Efficacy of antidepressants in relieving diabetic neuropathy pain: Amitriptyline vs desipramine, and fluoxetine vs placebo. Neurology 40 (Suppl 1): 437
Max MB, Kishore-Kumar R, Schafer SC, Meister B, Gracely RH, Smeller B, Dubner R (1991) Efficacy of desipramine in painful diabetic neuropathy: a placebo-controlled trial. Pain 45: 3–9
Peet M, Tienary P, Jaskari MO (1977) A comparison of the cardiac effects of mianserin and amitriptyline. Pharmakopsychiatrie 10: 309–312
Giardina E-GV, Bigger JT, Glassman AH, Perel JM, Kantor SJ (1979) The electrocardiographic and antiarrhytmic effects of imipramine hydrocloride at therapeutic plasma concentrations. Circulation 60: 1045–1052
Juan H (1977) Inhibition of algesic effect of bradykinin and acetylcholine by mepacrine. NS Arch Pharmacol 301: 23–27
Boulton AJM, Drury FJ, Clarke B, Ward JD (1982) Continuous subcutaneous insulin infusion in the management of painful diabetic neuropathy. Diabetes Care 5: 386–390
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Sindrup, S.H., Tuxen, C., Gram, L.F. et al. Lack of effect of mianserin on the symptoms of diabetic neuropathy. Eur J Clin Pharmacol 43, 251–255 (1992). https://doi.org/10.1007/BF02333018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02333018