Abstract
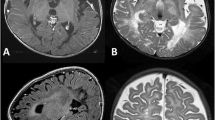
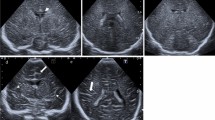
We describe three patients with Lowe (oculocerebrorenal) syndrome, emphasizing primarily the central nervous system and renal pathology. Using magnetic resonance imaging, we noted diffuse high T2 signals periventricularly, indicating significant white matter destruction, which may be responsible in part for the mental retardation, seizure disorder, hypotonia, and areflexia observed in the patients. In contrast to previously published reports, there was minimal renal tubular dysfunction; however, proteinuria was significantly increased in all patients. We believe that the observed proteinuria is primarily the result of glomerular pathology rather than renal tubular dysfunction and may represent a net loss of negative charges within the glomerular filter. This loss of charge may be linked to the increased excretion of glycosaminoglycans in the urine.
Similar content being viewed by others
References
Athreya BH, Schumacher HR, Getz HD, Norman ME, Borden S IV, Witzleben CL (1983) Arthropathy of Lowe's (oculocerebrorenal) syndrome. Arthritis Rheum 26: 728–735
Barnerjee AK, Allen IV, McKee P (1982) Oculo-cerebro-renal syndrome: failure to demonstrate specific neuropathological abnormalities in four cases. Ir J Med Sci 151:42–45
Bartsocas CS, Levy HL, Crawford JD, Thier SO (1969) A defect in intestinal amino acid transport in Lowe's syndrome. Am J Dis Child 117:93–95
Brodehl J (1978) The Fanconi syndrome. In: Edelmann CM (ed) Pediatric kidney disease. Little Brown & Co, Boston, pp 955–986
Charnas L, Berner J, Pezeshkpour GH, Dalakas M, Harper GS, Gahl WA (1988) MRI findings and peripheral neuropathy in Lowe syndrome. Neuropediatrics 19:7–9
Elliman D, Woodley A (1983) Tenosynovitis in Lowe syndrome. J Pediatr 103:1011
Gobernado JM, Lousa M, Gimeno A, Gonsalvez M (1984) Mitochondrial defects in Lowe's oculocerebrorenal syndrome. Arch Neurol 41:208–209
Habid R, Bargetyon E, Brissaud HE, Raynaud J, Ball JC de (1962) Constatations anatomiques chez un enfant atteint d'un syndrome de Lowe. Arch Fr Pediatr 19:945–960
Hambeaus L, Pallisgaard G, Kildeberg P (1970) The lowe syndrome: observations on the amino acid metabolism in a 2-year-old affected boy. Acta Pediatr Scand 59:631–636
Hayashi S, Nagata T, Kimura A, Tsurumi K (1978) Urinary excretion of acid glycosaminoglycans and hydroxyproline in a patient with oculo-cerebro-renal syndrome. Tohoku J Exp Med 126:215–223
Hayashi S, Nagata T, Kimura A, Tsurumi K (1978) Urinary acid glycosaminoglycans in a patient with oculo-cerebro-renal dyndrome. Tohoku J Exp Med 126:225–234
Hotgrewe JL, Kalen V (1986) Orthopedic manifestations of the Lowe (oculocerebrorenal) syndrome. J Pediatr Orthop 6:165–171
Jones KL (1988) Smith's recognizable patterns of human malformation, 4th edn. Saunders, Philadelphia
Kieras FJ, Houck GE, French JH, Wisniewski K (1984) Low sulfated glycosaminoglycans are excreted in patients with the Lowe syndrome. Biochem Med 31:201–210
Lowe CU, Terrey M, MacLachlan EA (1952) Organic aciduria, decreased renal ammonia production, hydrophthalmos, and mental retardation. Am J Dis Child 83:164–184
Martin JJ, Schlote W (1972) Central nervous system lesions in disorders of amino acid metabolism. J Neurol Sci 15:29–76
McKusick VA (1988) Mendelian inheritance in man, 8th edn. Johns Hopkins University Press, Baltimore, pp 1335–1336
O'Tuama LA, Laster DW (1987) Oculocerebrrenal syndrome: case report with CT and MRI correlation. AJNR 8:555–557
Rosenblatt D, Holmes LB (1974) Development of arthritis in Lowe's syndrome. J Pediatr 84:924–925
Schwartz R, Hall PW, Gabuzda GJ (1964) Metabolism of ornithine and other amino acids in cerebral-oculo-renal syndrome. Am J Med 36:778–786
Silver DN, Lewis RA, Nussbaum RL (1987) Mapping the Lowe oculocerebrorenal syndrome to Xq24-q26 by use of restriction fragment length polymorphisms. J Clin Invest 79:282–285
Silver Reilly D, Lewis RA, Ledbetter DH, Nussbaum RL (1988) Tightly linked flanking markers for the Lowe oculocerebrorenal syndrome, with application to carrier assessment. Am J Hum Genet 42:748–755
Suschke J, Murken JD (1969) Über die Ausscheidung saurer Mucopolysacchariden bei einem Kind mit Lowe-Syndrom. Monatsschr Kinderheilkd 117:412–414
Van Acker KJ, Roels H, Beelaerts W, Pasternack A, Valcke R (1967) The histologic lesions of the kidney in the oculo-cerebrorenal syndrome of Lowe. Nephron 4: 193–214
Wadelius C, Fagerholm P, Pettersson U, Annerén G (1989) Lowe oculocerebrorenal syndrome: DNA-based linkage of the gene to Xq24-q26, using tightly linked flanking markers and the correlation to lens examination in carrier diagnosis. Am J Hum Genet 44:241–247
Wisniewski KE, Kieras FJ, French JH, Houck GE, Ramos PL (1984) Ultrastructural, neurological and glycosaminoglycan abnormalities in Lowe syndrome. Ann Neurol 16:40–49
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Pueschel, S.M., Brem, A.S. & Nittoli, P. Central nervous system and renal investigations in patients with Lowe syndrome. Child's Nerv Syst 8, 45–48 (1992). https://doi.org/10.1007/BF00316562
Received:
Issue Date:
DOI: https://doi.org/10.1007/BF00316562