Addressing overweight and obesity is an important strategy in the primary and second prevention of disease including type 2 diabetes, hypertension, dyslipidemia, and cardiovascular disease [
3]. A sustained modest weight loss (approximately 5% to 10%) is associated with decreased risk of prediabetes, reductions in blood pressure, and improved lipids profiles [
4]. Thus, the questions of what are effective weight loss interventions, and what are realistic long-term outcomes, take on added importance for all health professionals counseling patients who are overweight/obese, as well as for the general public.
To answer these questions, we conducted a systematic review and meta-analysis of weight-loss intervention outcomes in studies with a minimum follow-up for 12 months [
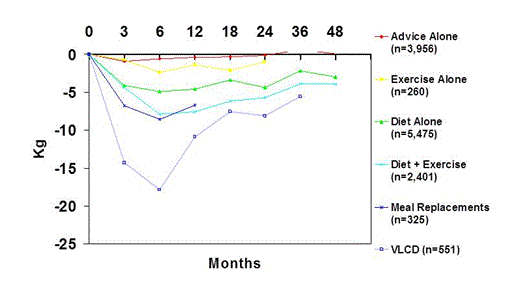
5]. A total of 80 studies (n=26,355 with 18,199 completers (69%)) were reviewed. Weight-loss studies were categorized into eight types of interventions: advice alone, diet alone, diet and exercise, exercise alone, meal replacements, very-low-energy diets, and weight -loss medications (orlistat and sibutramine). A mean weight loss of 7.9 kg (8.5%) was observed during the first six months from diet and exercise, meal replacements, and/or weight-loss medications with weight plateaus at approximately six months. In studies extending to 48 months, a mean 3.9 kg (4%) of weight loss was maintained with none of the groups experiencing weight regain to baseline. Participants who received diet alone experienced a mean weight loss at six months of 4.9 kg (5%), maintaining a mean weight loss of 4.6 to 4.4 to 3.0 kg (4.2%, 3.0%, 3.0%) at 12, 24, and 48 months, respectively. Very –low-energy diet use resulted in a major mean weight loss of 17.9 kg (16%) at six months followed by a rapid regain so that at 12 months the mean weight loss was 10.9 kg (10%) and by 36 months 5.6 kg (5%). Exercise alone, without a focus on food intake, was not very effective, resulting in a mean 2.4 kg (2.7%) weight loss at six months and a mean of 1.0 kg (1.0%) at 24 months. It should, of course, be remembered the results are a bell-shaped curve, with some participants experiencing greater weight loss (the ones remembered by health professionals and reported in ads and television shows) and some participants experiencing very minimal, if any, weight loss (the ones “forgotten” by health professionals!). Figure 1 illustrates mean weight loss per subject in the lifestyle weight loss intervention groups (diet alone, diet + exercise, meal replacements, very-low calorie diets, exercise alone) and the advice alone group.
The primary weight- loss intervention implemented in the intervention arms was a reduced energy, lower-fat eating plan. Several studies used some combination of low-carbohydrate, high-protein diets. However, at 12 months there were no differences in weight loss based on the macronutrient content of the eating plan implemented. Specific goals for physical activity were also implemented. Continuous or intermittent moderate intensity exercise of 30 to 40 minutes three to five days per week or 150 minutes per week of moderate intensity physical activity/exercise was recommended. In addition, basic weight-loss behavioral strategies were used in nearly all of the studies, which include self-monitoring, goal setting, stimulus control, reinforcement, and cognitive change. Study participants in the clinical trials also benefitted from the continued professional support they received.
Because weight loss plateaus at approximately six months, the emphasis of a weight-management program must evolve from a focus on reduced energy intake and regular physical activity for weight loss to a focus on reduced energy intake and regular physical activity for continued weight-loss maintenance [
6]. Health care professionals and participants often express frustration believing that if a reduced energy intake is maintained (or decreased even further as was done in some studies), weight loss should continue. There is no evidence that this occurs, even when weight-loss interventions are continued. However, if the weight loss interventions are discontinued, weight regain is likely to occur.
Individuals with obesity struggling to achieve and maintain weight loss are often not adequately aware of the biological adaptations that occur when they lose weight [
7]. Irrespective of starting weight, caloric restriction triggers several biological adaptations designed to prevent starvation [
8]. Weight is tightly regulated by neural, hormonal, and metabolic factors. Hormonal adaptations (decreased leptin, peptide YY, cholecystokinin, insulin and increased ghrelin, gastric inhibitory polypeptide, pancreatic polypeptide) that stimulate appetite and weight gain after diet-induced weight loss remain for at least one-year after the initial weight reduction [
9]. Weight loss also results in adaptive thermogenesis (decrease in resting metabolic rate) that has also been shown to be maintained for up to one year [
10]. Further evidence indicates that biological pressure to restore bodyweight to the highest-sustained lifetime levels gets stronger as weight loss increases [
11]. Therefore, weight maintenance strategies must be ongoing and take into account the fact that weight-loss maintenance is more difficult than weight loss.
It is, however, important to remind individuals struggling with weight that weight losses of 5% to 10% of initial bodyweight result in clinically meaningful risk reductions-prevention or delay of type 2 diabetes, decreases in blood pressure and circulating inflammatory markers (C-reactive protein and cytokines), and potential improvements in lipid levels, despite the fact that these weight loss goals might be disappointing to the individual [4].